Ch. 54 – Biliary System
Ch. 54 – Biliary System
Ch. 54 – Biliary System
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
1576 Section X Abdomen<br />
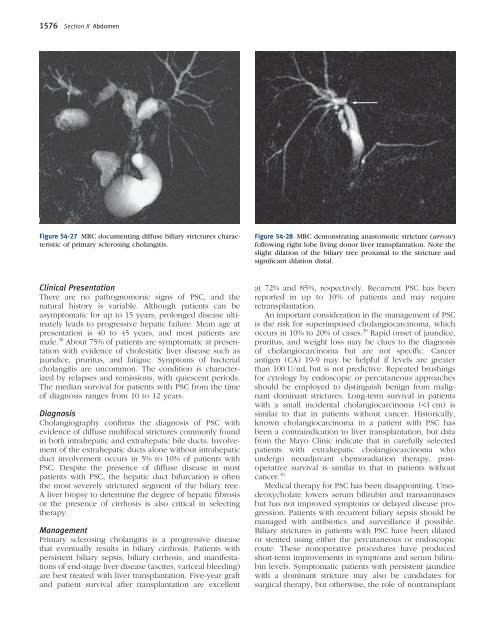
Figure <strong>54</strong>-27 MRC documenting diffuse biliary strictures characteristic<br />
of primary sclerosing cholangitis.<br />
Clinical Presentation<br />
There are no pathognomonic signs of PSC, and the<br />
natural history is variable. Although patients can be<br />
asymptomatic for up to 15 years, prolonged disease ultimately<br />
leads to progressive hepatic failure. Mean age at<br />
presentation is 40 to 45 years, and most patients are<br />
male. 38 About 75% of patients are symptomatic at presentation<br />
with evidence of cholestatic liver disease such as<br />
jaundice, pruritus, and fatigue. Symptoms of bacterial<br />
cholangitis are uncommon. The condition is characterized<br />
by relapses and remissions, with quiescent periods.<br />
The median survival for patients with PSC from the time<br />
of diagnosis ranges from 10 to 12 years.<br />
Diagnosis<br />
<strong>Ch</strong>olangiography confi rms the diagnosis of PSC with<br />
evidence of diffuse multifocal strictures commonly found<br />
in both intrahepatic and extrahepatic bile ducts. Involvement<br />
of the extrahepatic ducts alone without intrahepatic<br />
duct involvement occurs in 5% to 10% of patients with<br />
PSC. Despite the presence of diffuse disease in most<br />
patients with PSC, the hepatic duct bifurcation is often<br />
the most severely strictured segment of the biliary tree.<br />
A liver biopsy to determine the degree of hepatic fi brosis<br />
or the presence of cirrhosis is also critical in selecting<br />
therapy.<br />
Management<br />
Primary sclerosing cholangitis is a progressive disease<br />
that eventually results in biliary cirrhosis. Patients with<br />
persistent biliary sepsis, biliary cirrhosis, and manifestations<br />
of end-stage liver disease (ascites, variceal bleeding)<br />
are best treated with liver transplantation. Five-year graft<br />
and patient survival after transplantation are excellent<br />
Figure <strong>54</strong>-28 MRC demonstrating anastomotic stricture (arrow)<br />
following right lobe living donor liver transplantation. Note the<br />
slight dilation of the biliary tree proximal to the stricture and<br />
signifi cant dilation distal.<br />
at 72% and 85%, respectively. Recurrent PSC has been<br />
reported in up to 10% of patients and may require<br />
retransplantation.<br />
An important consideration in the management of PSC<br />
is the risk for superimposed cholangiocarcinoma, which<br />
occurs in 10% to 20% of cases. 39 Rapid onset of jaundice,<br />
pruritus, and weight loss may be clues to the diagnosis<br />
of cholangiocarcinoma but are not specifi c. Cancer<br />
antigen (CA) 19-9 may be helpful if levels are greater<br />
than 100 U/mL but is not predictive. Repeated brushings<br />
for cytology by endoscopic or percutaneous approaches<br />
should be employed to distinguish benign from malignant<br />
dominant strictures. Long-term survival in patients<br />
with a small incidental cholangiocarcinoma (