Ch. 54 – Biliary System
Ch. 54 – Biliary System
Ch. 54 – Biliary System
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
1584 Section X Abdomen<br />
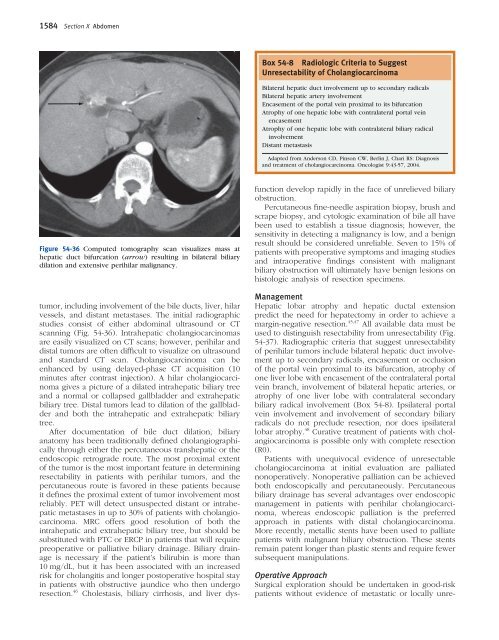
Figure <strong>54</strong>-36 Computed tomography scan visualizes mass at<br />
hepatic duct bifurcation (arrow) resulting in bilateral biliary<br />
dilation and extensive perihilar malignancy.<br />
tumor, including involvement of the bile ducts, liver, hilar<br />
vessels, and distant metastases. The initial radiographic<br />
studies consist of either abdominal ultrasound or CT<br />
scanning (Fig. <strong>54</strong>-36). Intrahepatic cholangiocarcinomas<br />
are easily visualized on CT scans; however, perihilar and<br />
distal tumors are often diffi cult to visualize on ultrasound<br />
and standard CT scan. <strong>Ch</strong>olangiocarcinoma can be<br />
enhanced by using delayed-phase CT acquisition (10<br />
minutes after contrast injection). A hilar cholangiocarcinoma<br />
gives a picture of a dilated intrahepatic biliary tree<br />
and a normal or collapsed gallbladder and extrahepatic<br />
biliary tree. Distal tumors lead to dilation of the gallbladder<br />
and both the intrahepatic and extrahepatic biliary<br />
tree.<br />
After documentation of bile duct dilation, biliary<br />
anatomy has been traditionally defi ned cholangiographically<br />
through either the percutaneous transhepatic or the<br />
endoscopic retrograde route. The most proximal extent<br />
of the tumor is the most important feature in determining<br />
resectability in patients with perihilar tumors, and the<br />
percutaneous route is favored in these patients because<br />
it defi nes the proximal extent of tumor involvement most<br />
reliably. PET will detect unsuspected distant or intrahepatic<br />
metastases in up to 30% of patients with cholangiocarcinoma.<br />
MRC offers good resolution of both the<br />
intrahepatic and extrahepatic biliary tree, but should be<br />
substituted with PTC or ERCP in patients that will require<br />
preoperative or palliative biliary drainage. <strong>Biliary</strong> drainage<br />
is necessary if the patient’s bilirubin is more than<br />
10 mg/dL, but it has been associated with an increased<br />
risk for cholangitis and longer postoperative hospital stay<br />
in patients with obstructive jaundice who then undergo<br />
resection. 46 <strong>Ch</strong>olestasis, biliary cirrhosis, and liver dys-<br />
Box <strong>54</strong>-8 Radiologic Criteria to Suggest<br />
Unresectability of <strong>Ch</strong>olangiocarcinoma<br />
Bilateral hepatic duct involvement up to secondary radicals<br />
Bilateral hepatic artery involvement<br />
Encasement of the portal vein proximal to its bifurcation<br />
Atrophy of one hepatic lobe with contralateral portal vein<br />
encasement<br />
Atrophy of one hepatic lobe with contralateral biliary radical<br />
involvement<br />
Distant metastasis<br />
Adapted from Anderson CD, Pinson CW, Berlin J, <strong>Ch</strong>ari RS: Diagnosis<br />
and treatment of cholangiocarcinoma. Oncologist 9:43-57, 2004.<br />
function develop rapidly in the face of unrelieved biliary<br />
obstruction.<br />
Percutaneous fi ne-needle aspiration biopsy, brush and<br />
scrape biopsy, and cytologic examination of bile all have<br />
been used to establish a tissue diagnosis; however, the<br />
sensitivity in detecting a malignancy is low, and a benign<br />
result should be considered unreliable. Seven to 15% of<br />
patients with preoperative symptoms and imaging studies<br />
and intraoperative fi ndings consistent with malignant<br />
biliary obstruction will ultimately have benign lesions on<br />
histologic analysis of resection specimens.<br />
Management<br />
Hepatic lobar atrophy and hepatic ductal extension<br />
predict the need for hepatectomy in order to achieve a<br />
margin-negative resection. 45,47 All available data must be<br />
used to distinguish resectability from unresectability (Fig.<br />
<strong>54</strong>-37). Radiographic criteria that suggest unresectability<br />
of perihilar tumors include bilateral hepatic duct involvement<br />
up to secondary radicals, encasement or occlusion<br />
of the portal vein proximal to its bifurcation, atrophy of<br />
one liver lobe with encasement of the contralateral portal<br />
vein branch, involvement of bilateral hepatic arteries, or<br />
atrophy of one liver lobe with contralateral secondary<br />
biliary radical involvement (Box <strong>54</strong>-8). Ipsilateral portal<br />
vein involvement and involvement of secondary biliary<br />
radicals do not preclude resection, nor does ipsilateral<br />
lobar atrophy. 48 Curative treatment of patients with cholangiocarcinoma<br />
is possible only with complete resection<br />
(R0).<br />
Patients with unequivocal evidence of unresectable<br />
cholangiocarcinoma at initial evaluation are palliated<br />
nonoperatively. Nonoperative palliation can be achieved<br />
both endoscopically and percutaneously. Percutaneous<br />
biliary drainage has several advantages over endoscopic<br />
management in patients with perihilar cholangiocarcinoma,<br />
whereas endoscopic palliation is the preferred<br />
approach in patients with distal cholangiocarcinoma.<br />
More recently, metallic stents have been used to palliate<br />
patients with malignant biliary obstruction. These stents<br />
remain patent longer than plastic stents and require fewer<br />
subsequent manipulations.<br />
Operative Approach<br />
Surgical exploration should be undertaken in good-risk<br />
patients without evidence of metastatic or locally unre-