Vol 44 # 2 June 2012 - Kma.org.kw
Vol 44 # 2 June 2012 - Kma.org.kw
Vol 44 # 2 June 2012 - Kma.org.kw
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
137<br />
Spinal Cord Demyelination in Biotinidase Deficiency: A Case Report<br />
<strong>June</strong> <strong>2012</strong><br />
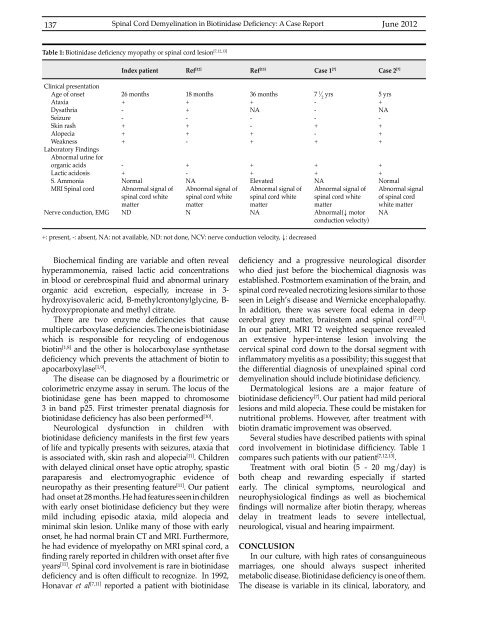
Table 1: Biotinidase deficiency myopathy or spinal cord lesion [7,12,13]<br />
Index patient<br />
Ref [12]<br />
Ref [13]<br />
Case 1 [7]<br />
Case 2 [7]<br />
Clinical presentation<br />
Age of onset<br />
Ataxia<br />
Dysathria<br />
Seizure<br />
Skin rash<br />
Alopecia<br />
Weakness<br />
Laboratory Findings<br />
Abnormal urine for<br />
<strong>org</strong>anic acids<br />
Lactic acidosis<br />
S. Ammonia<br />
MRI Spinal cord<br />
Nerve conduction, EMG<br />
26 months<br />
+<br />
-<br />
-<br />
+<br />
+<br />
+<br />
-<br />
+<br />
Normal<br />
Abnormal signal of<br />
spinal cord white<br />
matter<br />
ND<br />
18 months<br />
+<br />
+<br />
-<br />
+<br />
+<br />
-<br />
+<br />
-<br />
NA<br />
Abnormal signal of<br />
spinal cord white<br />
matter<br />
N<br />
36 months<br />
+<br />
NA<br />
-<br />
-<br />
+<br />
+<br />
+<br />
+<br />
Elevated<br />
Abnormal signal of<br />
spinal cord white<br />
matter<br />
NA<br />
7 1 ⁄ 2<br />
yrs<br />
-<br />
-<br />
-<br />
+<br />
-<br />
+<br />
+<br />
+<br />
NA<br />
Abnormal signal of<br />
spinal cord white<br />
matter<br />
Abnormal(↓ motor<br />
conduction velocity)<br />
5 yrs<br />
+<br />
NA<br />
-<br />
+<br />
+<br />
+<br />
+<br />
+<br />
Normal<br />
Abnormal signal<br />
of spinal cord<br />
white matter<br />
NA<br />
+: present, -: absent, NA: not available, ND: not done, NCV: nerve conduction velocity, ↓: decreased<br />
Biochemical finding are variable and often reveal<br />
hyperammonemia, raised lactic acid concentrations<br />
in blood or cerebrospinal fluid and abnormal urinary<br />
<strong>org</strong>anic acid excretion, especially, increase in 3-<br />
hydroxyisovaleric acid, B-methylcrontonylglycine, B-<br />
hydroxypropionate and methyl citrate.<br />
There are two enzyme deficiencies that cause<br />
multiple carboxylase deficiencies.Theoneisbiotinidase<br />
which is responsible for recycling of endogenous<br />
biotin [1,8] and the other is holocarboxylase synthetase<br />
deficiency which prevents the attachment of biotin to<br />
apocarboxylase [1,9] .<br />
The disease can be diagnosed by a flourimetric or<br />
colorimetric enzyme assay in serum. The locus of the<br />
biotinidase gene has been mapped to chromosome<br />
3 in band p25. First trimester prenatal diagnosis for<br />
biotinidase deficiency has also been performed [10] .<br />
Neurological dysfunction in children with<br />
biotinidase deficiency manifests in the first few years<br />
of life and typically presents with seizures, ataxia that<br />
is associated with, skin rash and alopecia [11] . Children<br />
with delayed clinical onset have optic atrophy, spastic<br />
paraparesis and electromyographic evidence of<br />
neuropathy as their presenting feature [11] . Our patient<br />
had onset at 28 months. He had features seen in children<br />
with early onset biotinidase deficiency but they were<br />
mild including episodic ataxia, mild alopecia and<br />
minimal skin lesion. Unlike many of those with early<br />
onset, he had normal brain CT and MRI. Furthermore,<br />
he had evidence of myelopathy on MRI spinal cord, a<br />
finding rarely reported in children with onset after five<br />
years [11] . Spinal cord involvement is rare in biotinidase<br />
deficiency and is often difficult to recognize. In 1992,<br />
Honavar et al [7,11] reported a patient with biotinidase<br />
deficiency and a progressive neurological disorder<br />
who died just before the biochemical diagnosis was<br />
established. Postmortem examination of the brain, and<br />
spinal cord revealed necrotizing lesions similar to those<br />
seen in Leigh’s disease and Wernicke encephalopathy.<br />
In addition, there was severe focal edema in deep<br />
cerebral grey matter, brainstem and spinal cord [7,11] .<br />
In our patient, MRI T2 weighted sequence revealed<br />
an extensive hyper-intense lesion involving the<br />
cervical spinal cord down to the dorsal segment with<br />
inflammatory myelitis as a possibility; this suggest that<br />
the differential diagnosis of unexplained spinal cord<br />
demyelination should include biotinidase deficiency.<br />
Dermatological lesions are a major feature of<br />
biotinidase deficiency [7] . Our patient had mild perioral<br />
lesions and mild alopecia. These could be mistaken for<br />
nutritional problems. However, after treatment with<br />
biotin dramatic improvement was observed.<br />
Several studies have described patients with spinal<br />
cord involvement in biotinidase difficiency. Table 1<br />
compares such patients with our patient [7,12,13] .<br />
Treatment with oral biotin (5 - 20 mg/day) is<br />
both cheap and rewarding especially if started<br />
early. The clinical symptoms, neurological and<br />
neurophysiological findings as well as biochemical<br />
findings will normalize after biotin therapy, whereas<br />
delay in treatment leads to severe intellectual,<br />
neurological, visual and hearing impairment.<br />
CONCLUSION<br />
In our culture, with high rates of consanguineous<br />
marriages, one should always suspect inherited<br />
metabolic disease. Biotinidase deficiency is one of them.<br />
The disease is variable in its clinical, laboratory, and