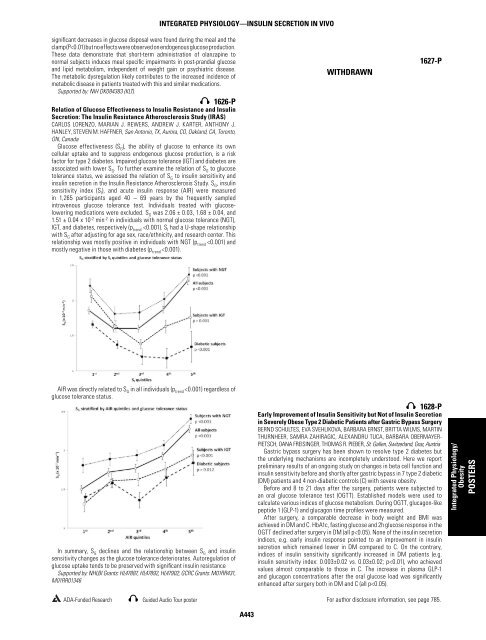
signifi cant decreases in glucose disposal were found during the meal and the clamp (P
Integrated Physiology/ Obesity POSTERS Despite of a markedly enhanced GLP-1 response there was no improvement in insulin secretion but an unexpected increase in glucagon levels during the OGTT shortly after gastric bypass surgery. While gastric bypass surgery in the short-term appears to leave beta cell function unaffected it obviously exerts a strong stimulating effect on alpha cell function. Collectively, our data speak against a major contribution of incretin effects to the early improvement in glucose metabolism after gastric bypass surgery which appears to rely primarily on enhanced insulin sensitivity. DM C pre-operative post-operative pre-operative post-operative GLP-1 AUC (pg/ml/min) 0.56±0.34 2.61±0.96 0.46±0.35 3.58±1.72 Glucagon AUC (pg/ml/min) 11.27±3.10 52.20±16.19 10.11±4.22 53.36±12.14 Supported by: EFSD/MSD Clinical Research Grant 2009 & 1629-P Impaired Insulinotropic Effect of Both GLP-1 and GIP Can Be Induced in Healthy Normal Glucose Tolerant Subjects KATRINE B. HANSEN, TINA VILSBØLL, JONATAN I. BAGGER, JENS J. HOLST, FILIP K. KNOP, Glostrup, Denmark, Gentofte, Denmark, Copenhagen, Denmark The insulinotropic effect of the incretin hormones glucose-dependent insulinotropic polypeptide (GIP) and glucagon-like peptide-1 (GLP-1) is impaired in patients with type 2 diabetes. It remains unclear whether this impairment can be induced temporarily in healthy subjects by a short period of glucose homeostatic dysregulation. We aimed to investigate the insulinotropic effect of GIP and GLP-1 compared to placebo (saline) before and after 12 days of glucose homeostatic dysregulation in healthy subjects. The insulinotropic effect was measured using hyperglycemic clamps and infusion of physiological doses of GIP, GLP-1 or saline in 10 healthy Caucasian males (age: 25±1 years (mean±SEM); BMI: 23±1kg/m 2 ; HbA 1 c: 5.4±0.1%; no family history of diabetes) before and after intervention using high calorie diet, sedentary lifestyle and administration of prednisolone (37.5 mg/day) for 12 days. The intervention resulted in insulin resistance (IR) according to the homeostatic model assessment (1.2±0.2 vs 2.6±0.5, P=0.01) and glucose tolerance deteriorated as assessed by the area under curve (AUC) for plasma glucose during 75 g-OGTT (730±30 vs. 846±57mM×2h, P=0.021). The subjects compensated for the induced IR by signifi cantly increasing their post intervention insulin responses during saline infusion by 2.9±0.5 fold; signifi cantly (P=0.001) more than during GIP or GLP-1 infusions (1.78±0.3 and 1.38±0.3, P=NS). These data show that impairment of the insulinotropic effect of both GIP and GLP-1 can be induced in healthy male subjects without risk factors for type 2 diabetes. This fi nding indicates that the impaired insulinotropic effect of the incretin hormones observed in type 2 diabetes is a consequence of insulin resistance and glucose intolerance rather than a primary event causing type 2 diabetes. Supported by: EFSD/Novartis Grant & 1630-P Pioglitazone (PIO) Does Not Enhance Glucose-Dependent Insulinotropic Peptide (GIP) Stimulated Insulin Secretion in Subjects with Well-Controlled T2DM WILLIAM G. THARP, OLGA SIDELEVA, DARIUSH ELAHI, COURTNEY LEDGER, RHONDA MAPLE, RICHARD PRATLEY, Burlington, VT, Baltimore, MD Dysregulation of incretin action contributes to hyperglycemia in Type 2 diabetes(T2DM). GIP stimulated insulin secretion(GIP-SIS) is markedly blunted, possibly due to down-regulation of GIP receptor in β-cells by chronic hyperglycemia. The promoter of GIP receptor contains a PPAR response element. We hypothesized that treatment with PIO, a potent PPARγ agonist, would improve GIP-SIS in subjects with T2DM. Twenty four subjects (12M/12F, age 58.7+10.6, BMI 33.4+8.1) with well controlled T2DM (A1c