programma & abstracts - Nederlandse Vereniging voor Radiologie
programma & abstracts - Nederlandse Vereniging voor Radiologie
programma & abstracts - Nederlandse Vereniging voor Radiologie
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Neuro- en Hoofdhals radiologie 9<br />
Results: Ten of hundred included patients suffered from<br />
recurrent ipsilateral clinical ischemic events (9 TIAs and 1<br />
ischemic stroke). The presence of IPH was associated with<br />
recurrence (Pearson Chi-Square= 7.373, P=0.007). Patients<br />
with recurrent events also had plaques with larger LRNC<br />
volume and larger maximum vessel wall thickness, although<br />
these findings were borderline significant (P=0.032 and<br />
P=0.055, respectively). Other MRI-based parameters were<br />
not related to recurrent ischemic events.<br />
Conclusion: The results of this study indicate that the<br />
presence of IPH, larger LRNC volume, and larger maximum<br />
vessel wall thickness of carotid plaques are associated with<br />
recurrent TIA and ischemic stroke. Assessment of carotid<br />
plaque characteristics by MRI may help identifying high-risk<br />
patients, which could improve patient selection for carotid<br />
endarterectomy or stenting.<br />
O9.3<br />
CAROTID PLAQUE MORPHOLOGY AND<br />
ISCHEMIC VASCULAR BRAIN DISEASE ON<br />
MRI<br />
Q.J.A. van den Bouwhuijsen, M.W. Vernooij, W.J. Niessen,<br />
G.P. Krestin, M.A. Ikram, J.C.M. Witteman, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Vulnerable plaque components in carotid arteries<br />
can be detected non-invasively with magnetic resonance<br />
imaging (MRI). In asymptomatic persons, the relation between<br />
carotid plaque composition and vascular brain disease<br />
is not well studied. We studied the association between<br />
carotid atherosclerotic plaque characteristics and ischemic<br />
brain disease on MRI.<br />
Methods: From the population-based Rotterdam Study, 952<br />
participants with carotid wall thickening on ultrasound >2.5<br />
mm underwent both carotid MRI and brain MRI. Maximum<br />
carotid wall thickening, degree of stenosis and presence of<br />
intraplaque hemorrhage, lipid core and calcification were<br />
assessed in both carotid arteries. Associations between<br />
plaque characteristics and white matter lesions (WMLs),<br />
lacunar and cortical infarcts were investigated per<br />
participant and additionally per carotid artery. Analysis were<br />
adjusted for cardiovascular risk factors.<br />
Results: Carotid stenosis (OR per 10% stenosis increase<br />
1.2 95% confidence interval (1.0-1.4), maximum carotid<br />
wall thickness (per mm increase 1.3,1.1-1.6) en presence of<br />
intraplaque hemorrhage (1.9,1.1-3.3), were all found to be<br />
significantly associated with presence of cortical infarcts,<br />
both in the participant based analysis and in the carotid<br />
artery based analysis. There were no associations between<br />
any plaque characteristics and presence of lacunar infarcts.<br />
In the subject based analysis maximum plaque thickness,<br />
presence of intraplaque hemorrhage and calcification were<br />
associated with WML-volume. In the artery based analysis<br />
only the association for calcifications remained.<br />
Conclusion: Presence of carotid intraplaque hemorrhage<br />
and measures of carotid plaque size are independently associated<br />
with cortical infarcts, but not with lacunar infarcts.<br />
Plaque calcification, but not vulnerable plaque components,<br />
is related to WML volume.<br />
Clinical relevance: This MRI study gives insight into the<br />
importance of atherosclerotic plaque composition, also in<br />
small plaques, for development of ischemic brain disease.<br />
O9.4<br />
A COMPUTER BASED DIAGNOSTIC<br />
SYSTEM TO FACILITATE THE EARLY AND<br />
DIFFERENTIAL DIAGNOSIS OF DEMENTIA<br />
B. Jasperse, H.A. Vrooman, M. Koek, M.W. Vernooij,<br />
R. de Boer, F. van der Lijn, M.A. Ikram, M. Smits,<br />
W. Niessen, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Patterns of brain atrophy, hippocampal atrophy and<br />
vascular changes, as visualized on brain-MRI, play an important<br />
role in determining the underlying cause of dementia<br />
syndromes. The visual interpretation of these pathological<br />
changes can be very challenging due to intercurrent agerelated<br />
brain changes.To facilitate the distinction between<br />
abnormal and ‘normal age-related’ brain changes, we<br />
developed an automated system that provides individualspecific<br />
lobar brain volumes, hippocampal volumes and white<br />
matter lesion volume taking into account age- and sex-specific<br />
reference data from a ‘healthy’ aging population.<br />
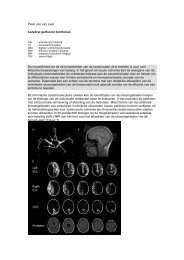
Methods and Materials: Automated brain tissue segmentation<br />
and atlas-based registration is performed on T1, T2<br />
and FLAIR MR-images, generating lobar brain volumes, hippocampal<br />
volumes and white matter lesion volume. For each<br />
resulting volume, reference curves are used to generate<br />
age- and sex-specific percentile values. The results are then<br />
presented in an on-line viewer to interpret the quality of tissue<br />
and structure segmentation and the quantitative results.<br />
Reference curves are generated from 867 healthy aging<br />
individuals (age-range (years): 61-91, Male/female-ratio (N):<br />
425/422).<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
63