The eligibility and enrollment rules for the U
The eligibility and enrollment rules for the U
The eligibility and enrollment rules for the U
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Retiree Health Care SPD Effective January 1, 2012<br />
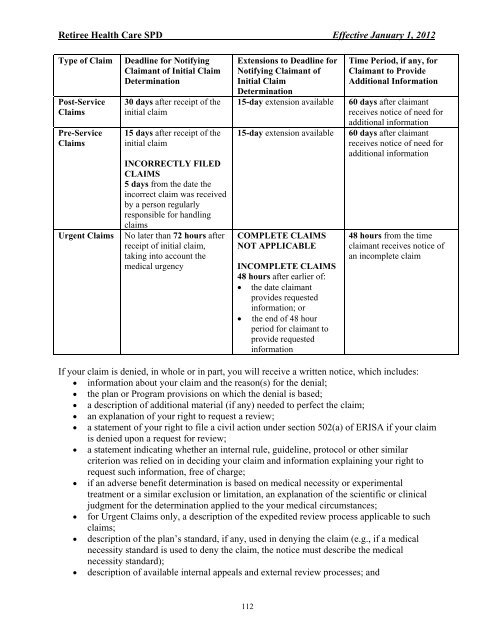
Type of Claim<br />
Post-Service<br />
Claims<br />
Pre-Service<br />
Claims<br />
Urgent Claims<br />
Deadline <strong>for</strong> Notifying<br />
Claimant of Initial Claim<br />
Determination<br />
30 days after receipt of <strong>the</strong><br />
initial claim<br />
15 days after receipt of <strong>the</strong><br />
initial claim<br />
INCORRECTLY FILED<br />
CLAIMS<br />
5 days from <strong>the</strong> date <strong>the</strong><br />
incorrect claim was received<br />
by a person regularly<br />
responsible <strong>for</strong> h<strong>and</strong>ling<br />
claims<br />
No later than 72 hours after<br />
receipt of initial claim,<br />
taking into account <strong>the</strong><br />
medical urgency<br />
Extensions to Deadline <strong>for</strong><br />
Notifying Claimant of<br />
Initial Claim<br />
Determination<br />
15-day extension available<br />
15-day extension available<br />
COMPLETE CLAIMS<br />
NOT APPLICABLE<br />
INCOMPLETE CLAIMS<br />
48 hours after earlier of:<br />
• <strong>the</strong> date claimant<br />
provides requested<br />
in<strong>for</strong>mation; or<br />
• <strong>the</strong> end of 48 hour<br />
period <strong>for</strong> claimant to<br />
provide requested<br />
in<strong>for</strong>mation<br />
Time Period, if any, <strong>for</strong><br />
Claimant to Provide<br />
Additional In<strong>for</strong>mation<br />
60 days after claimant<br />
receives notice of need <strong>for</strong><br />
additional in<strong>for</strong>mation<br />
60 days after claimant<br />
receives notice of need <strong>for</strong><br />
additional in<strong>for</strong>mation<br />
48 hours from <strong>the</strong> time<br />
claimant receives notice of<br />
an incomplete claim<br />
If your claim is denied, in whole or in part, you will receive a written notice, which includes:<br />
• in<strong>for</strong>mation about your claim <strong>and</strong> <strong>the</strong> reason(s) <strong>for</strong> <strong>the</strong> denial;<br />
• <strong>the</strong> plan or Program provisions on which <strong>the</strong> denial is based;<br />
• a description of additional material (if any) needed to perfect <strong>the</strong> claim;<br />
• an explanation of your right to request a review;<br />
• a statement of your right to file a civil action under section 502(a) of ERISA if your claim<br />
is denied upon a request <strong>for</strong> review;<br />
• a statement indicating whe<strong>the</strong>r an internal rule, guideline, protocol or o<strong>the</strong>r similar<br />
criterion was relied on in deciding your claim <strong>and</strong> in<strong>for</strong>mation explaining your right to<br />
request such in<strong>for</strong>mation, free of charge;<br />
• if an adverse benefit determination is based on medical necessity or experimental<br />
treatment or a similar exclusion or limitation, an explanation of <strong>the</strong> scientific or clinical<br />
judgment <strong>for</strong> <strong>the</strong> determination applied to <strong>the</strong> your medical circumstances;<br />
• <strong>for</strong> Urgent Claims only, a description of <strong>the</strong> expedited review process applicable to such<br />
claims;<br />
• description of <strong>the</strong> plan’s st<strong>and</strong>ard, if any, used in denying <strong>the</strong> claim (e.g., if a medical<br />
necessity st<strong>and</strong>ard is used to deny <strong>the</strong> claim, <strong>the</strong> notice must describe <strong>the</strong> medical<br />
necessity st<strong>and</strong>ard);<br />
• description of available internal appeals <strong>and</strong> external review processes; <strong>and</strong><br />
112