Eble JN, Sauter G., Epstein JI, Sesterhenn IA - iarc
Eble JN, Sauter G., Epstein JI, Sesterhenn IA - iarc
Eble JN, Sauter G., Epstein JI, Sesterhenn IA - iarc
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Differential diagnoses<br />
Differential diagnoses include, among the<br />
germ cell tumours, seminoma, solid type<br />
of yolk sac tumour, and choriocarcinoma.<br />
Among other tumours anaplastic large<br />
cell lymphoma, malignant Sertoli cell<br />
tumour and metastases are considerations.<br />
The age of the patient, microscopic<br />
examination of representative sections<br />
from the tumour including all growth patterns,<br />
and a small panel of immunohistochemical<br />
stains yields the correct<br />
diagnosis in the majority of the cases.<br />
Fig. 4.30 Embryonal carcinoma. Transverse ultrasound<br />
image of the testis (cursors) shows an ill<br />
defined, irregular, heterogeneous mass (arrows).<br />
ing abnormal forms. Syncytiotrophoblastic<br />
cells may occur scattered among<br />
the tumour cells as single cells or in small<br />
cell groups. Cells at the periphery of the<br />
solid tumour formations may appear<br />
degenerated, smudged or apoptotic<br />
resulting in a biphasic pattern that may<br />
mimic choriocarcinoma.<br />
The stroma that varies from scant within<br />
the solid formations, to more abundant at<br />
the periphery of the tumour is usual<br />
fibrous, more or less cellular and with or<br />
without lymphocytic infiltration. Eosinophils<br />
are rarely present as is granulomatous<br />
reaction.<br />
In the adjacent testicular tissue intratubular<br />
embryonal carcinoma is often present,<br />
and is often more or less necrotic,<br />
and sometimes calcified. In the surrounding<br />
tissue vascular and lymphatic<br />
invasion are also common and should be<br />
carefully distinguished from the intratubular<br />
occurrence and from artificial<br />
implantation of tumour cells into vascular<br />
spaces during handling of the specimen.<br />
Loose, "floating" tumour cells in vascular<br />
spaces, usually associated with surface<br />
implants of similar cells should be considered<br />
artefactual.<br />
Fig. 4.31 Embryonal carcinoma. The tumour is<br />
fleshy and has foci of haemorrhage and necrosis.<br />
Immunoprofile<br />
Embryonal carcinoma contains a number<br />
of immunohistochemical markers reflecting<br />
embryonic histogenesis but the<br />
majority have hitherto not been very useful<br />
diagnostically. CD30 can be demonstrated<br />
in many cases {2202}.<br />
Cytokeratins of various classes are present<br />
while epithelial membrane antigen<br />
(EMA) and carcinoembryonic antigen<br />
(CEA) and vimentin can usually not be<br />
demonstrated {1894}. Placental alkaline<br />
phosphatase (PLAP) occurs focally as a<br />
membranous and/or cytoplasmic staining<br />
{1615}. Many embryonal carcinomas<br />
are strongly positive for TP53 in up to<br />
50% of the tumour cells {2667}. AFP may<br />
occur in scattered cells {1196,1198}.<br />
Human placental lactogen (HPL) is occasionally<br />
found focally in the tumour cells<br />
{1198,1807}. HCG occurs in the syncytiotrophoblastic<br />
cells, which may be<br />
present in the tumour, but not in the<br />
embryonal carcinoma cells and the same<br />
applies to pregnancy specific ß 1<br />
glycoprotein<br />
(SP1) {1807}.<br />
Ultrastructure<br />
Ultrastructural examinations have not<br />
proven to be diagnostically useful<br />
although it may differentiate embryonal<br />
carcinoma from seminoma and glandular<br />
like pattern of embryonal carcinoma from<br />
somatic type adenocarcinomas.<br />
Prognosis<br />
The most important prognostic factor is<br />
clinical tumour stage. In general, the<br />
tumour spread is lymphatic, first to the<br />
retroperitoneal lymph nodes and subsequently<br />
to the mediastinum. Haematogeneous<br />
spread to the lung may also be<br />
seen. Patients with pure embryonal carcinoma<br />
and with vascular invasion tend<br />
to have higher stage disease {1200}. This<br />
is emphasized by studies defining high<br />
risk patients as those with pure embryonal<br />
carcinoma, predominant embryonal<br />
carcinoma, embryonal carcinoma unassociated<br />
with teratoma, and/or<br />
tumours with vascular/lymphatic invasion<br />
and advanced local stage {1803,1817}.<br />
Yolk sac tumour<br />
Definition<br />
A tumour characterized by numerous patterns<br />
that recapitulate the yolk sac, allantois<br />
and extra embryonic mesenchyme.<br />
ICD-O code 9071/3<br />
Synonym<br />
Endodermal sinus tumour, orchioblastoma.<br />
Epidemiology<br />
In the testis yolk sac tumour (YST) is<br />
seen in two distinct age groups, infants<br />
and young children and postpubertal<br />
males. In children, it is the most common<br />
testicular neoplasm {1274} and occurs in<br />
all races. It is less common in Blacks,<br />
Native Americans, and in Indians {490,<br />
A<br />
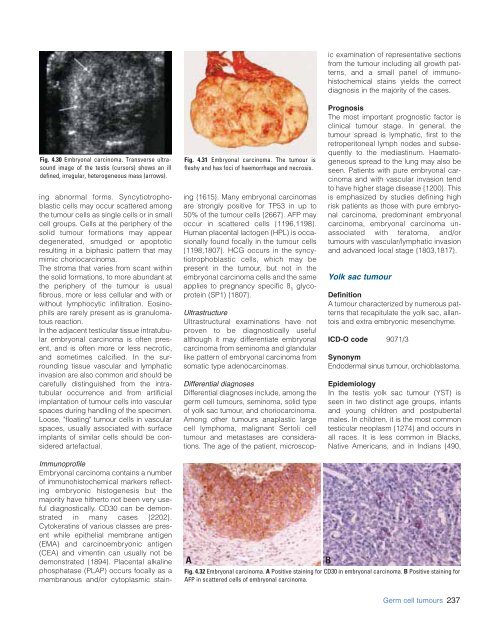
Fig. 4.32 Embryonal carcinoma. A Positive staining for CD30 in embryonal carcinoma. B Positive staining for<br />
AFP in scattered cells of embryonal carcinoma.<br />
B<br />
Germ cell tumours 237