10.- Bjordal JM, Ljunggren AE, Klovning A, Slørdal L. Non-steroidal anti-inflammatory drugs, including cyclo-oxygenase-2 inhibitors, in osteoarthritic knee pain: metaanalysis of randomised placebo controlled trials. BMJ. <strong>20</strong>04;329:1317. 11.- Zhang W, Nuki G, Moskowitz RW, Abramson S, Altman RD, Arden NK, et al. OARSI recommendations for the management of hip and knee osteoarthritis. <strong>Osteo</strong>arthr Cartil [Internet]. <strong>20</strong>10;18:476–99. 12.- da Costa BR, Reichenbach S, Keller N, Nartey L,Wandel S, Jüni P, et al. Effectiveness of non-steroidal anti-inflammatory drugs for the treatment of pain in knee and hip osteoarthritis: a network metaanalysis. Lancet (Lond, Engl). <strong>20</strong>17;390:e21–33. 13.- Sostres C, Gargallo CJ, Lanas A. Nonsteroidal anti-inflammatory drugs and upper and lower gastrointestinal mucosal damage. Arthritis Res Ther. <strong>20</strong>13;15(Suppl 3):S3. 14.- Al-Saeed A. Gastrointestinal and cardiovascular risk of nonsteroidal anti-inflammatory drugs. Oman Med J. <strong>20</strong>11;26:385–91. 15.- Krijthe BP, Heeringa J, Hofman A, Franco OH, Stricker BH. Nonsteroidal anti-inflammatory drugs and the risk of atrial fibrillation: a population-based follow-up study. BMJ Open [Internet]. <strong>20</strong>14 [cited <strong>20</strong>18 Sep 12];4:e004059. 16.- Jówiak-Bebenista M, Nowak JZ. Paracetamol: mechanism of action, applications and safety concern. Acta Pol Pharm [Internet]. <strong>20</strong>14;71:11–23. 17.- Towheed T, Maxwell L, Judd M, Catton M, Hochberg MC, Wells GA. Acetaminophen for osteoarthritis. Cochrane Database Syst Rev. <strong>20</strong>06;CD004257. 18.- Jaeschke H. Acetaminophen: dose-dependent drug hepatotoxicity and acute liver failure in patients. Dig Dis. <strong>20</strong>15;33:464–71. 19.- Abou-Raya S, Abou-Raya A, Helmii M. Duloxetine for the management of pain in older adults with knee osteoarthritis: randomized placebo-controlled trial. Age Ageing. <strong>20</strong>12;41:646–52. <strong>20</strong>.- Frakes EP, Risser RC, Ball TD, Hochberg MC, Wohlreich MM. Duloxetine added to oral nonsteroidal anti-inflammatory drugs for treatment of knee pain due to osteoarthritis: results of a randomized, double-blind, placebo-controlled trial. Curr Med Res Opin. <strong>20</strong>11;27:2361–72. 21.- Citrome L, Weiss–Citrome A. A systematic review of duloxetine for osteoarthritic pain: what is the number needed to treat, number needed to harm, and likelihood to be helped or harmed? Postgrad Med. <strong>20</strong>12;124:83–93. 22.- Guedes V, Castro JP, Brito I. Topical capsaicin for pain in osteoarthritis: a literature review. Reumatol Clin. <strong>20</strong>18;14:40–5. 23.- Yi P, Pryzbylkowski P. Opioid induced hyperalgesia. Pain Med. <strong>20</strong>15;16(Suppl 1):S32–6. 24.- Brat GA, Agniel D, Beam A, Yorkgitis B, Bicket M, Homer M, et al. Postsurgical prescriptions for opioid naive patients and association with overdose and misuse: retrospective cohort study. BMJ [Internet]. <strong>20</strong>18 [cited <strong>20</strong>18 Sep 11];j5790. 25.- Karsdal MA, Michaelis M, Ladel C, Siebuhr AS, Bihlet AR, Andersen JR, et al. Disease-modifying treatments for osteoarthritis (DMOADs) of the knee and hip: lessons learned from failures and opportunities for the future. <strong>Osteo</strong>arthr Cartil. <strong>20</strong>16;24:<strong>20</strong>13–21. 26.- McAlindon TE, LaValley MP, Gulin JP, Felson DT. Glucosamine and chondroitin for treatment of osteoarthritis: a systematic quality assessment and meta-analysis. JAMA. <strong>20</strong>00;283:1469–75. 27.- Singh JA, Noorbaloochi S, MacDonald R, Maxwell LJ. Chondroitin for osteoarthritis. In: Singh JA, editor. Cochrane database syst rev. Chichester: Wiley; <strong>20</strong>15. p. CD005614. 28.- Hochberg MC, Martel-Pelletier J, Monfort J, Möller I, Castillo JR, Arden N, et al. Combined chondroitin sulfate and glucosamine for painful knee osteoarthritis: a multicentre, randomised, double-blind, non-inferiority trial versus celecoxib. Ann Rheum Dis. <strong>20</strong>16;75:37–44. 29.- Fransen M, Agaliotis M, Nairn L, Votrubec M, Bridgett L, Su S, et al. Glucosamine and chondroitin for knee osteoarthritis: a double blind, randomized, placebocontrolled clinical trial evaluating single and combination regimens. Ann Rheum Dis. <strong>20</strong>15;74:851–8. 30.- Hart LE. In knee OA, intraarticular triamcinolone increased cartilage loss and did not differ from saline for knee pain. Ann InternMed. <strong>20</strong>17;167:JC27. 31.- Wang C-T, Lin J, Chang C-J, Lin Y-T, Hou S-M. Therapeutic effects of hyaluronic acid on osteoarthritis of the knee. A metaanalysis of randomized controlled trials. J Bone Joint Surg Am. <strong>20</strong>04;86–A:538–45. 32.- Patel S, Dhillon MS, Aggarwal S, Marwaha N, Jain A. Treatment with platelet-rich plasma is more effective than placebo for knee osteoarthritis: a prospective, double-blind, randomized trial. Am J Sports Med. <strong>20</strong>13;41:356–64. 33.- Mullard A. Drug developers reboot anti-NGF pain programmes. Nat Rev Drug Discov. <strong>20</strong>15;14:297–8. 34.- Schnitzer TJ, Marks JA. A systematic review of the efficacy and general safety of antibodies to NGF in the treatment of OA of the hip or knee. <strong>Osteo</strong>arthr Cartil. <strong>20</strong>15;23:S8–17. 35.- Schnitzer TJ, Ekman EF, Spierings ELH, Greenberg HS, Smith MD, BrownMT, et al. Efficacy and safety of tanezumab monotherapy or combined with nonsteroidal anti-inflammatory drugs in the treatment of knee or hip osteoarthritis pain. Ann Rheum Dis. <strong>20</strong>15;74:1<strong>20</strong>2–11. 36.- Kan S-L, Li Y, Ning G-Z, Yuan Z-F, Chen L-X, Bi M-C, et al. Tanezumab for patients with osteoarthritis of the knee: a meta-analysis. PLoS One. <strong>20</strong>16;11:e0157105. 37.- Chen J, Li J, Li R,Wang H, Yang J, Xu J, et al. Efficacy and safety of tanezumab on osteoarthritis knee and hip pains: a meta-analysis of randomized controlled trials. Pain Med. <strong>20</strong>16;18:pnw262. 38.- Miller RE, Block JA, Malfait A-M. What is new in pain modification in osteoarthritis? Rheumatology. <strong>20</strong>18;57:iv99–iv107. 39.- Emery EC, Luiz AP, Wood JN. Na v 1.7 and other voltage-gated sodium channels as drug targets for pain relief. Expert Opin Ther Targets. <strong>20</strong>16;<strong>20</strong>:975–83. 40.- Ding H, Kiguchi N, Yasuda D, Daga PR, PolgarWE, Lu JJ, et al. A bifunctional nociceptin and mu opioid receptor agonist is analgesic without opioid side effects in nonhuman primates. Sci Transl Med. <strong>20</strong>18;10:eaar3483. OSTEO <strong>360</strong> 60 Novedades en patología osteomioarticular
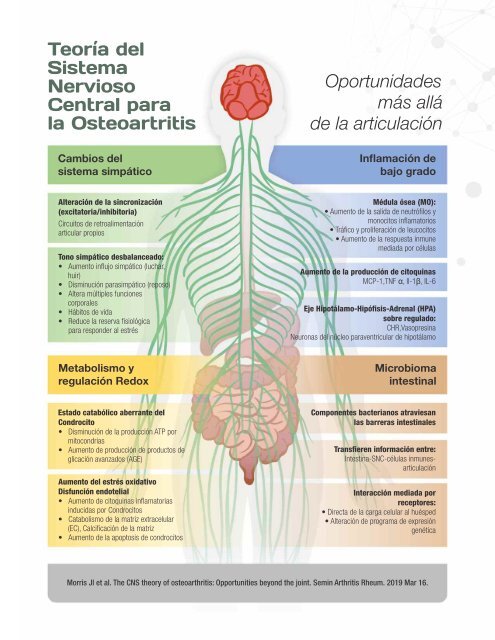
Teoría del Sistema Nervioso Central para la <strong>Osteo</strong>artritis Cambios del sistema simpático Oportunidades más allá de la articulación Inflamación de bajo grado Alteración de la sincronización (excitatoria/inhibitoria) Circuitos de retroalimentación articular propios Tono simpático desbalanceado: • Aumento influjo simpático (luchar, huir) • Disminución parasimpático (reposo) • Altera múltiples funciones corporales • Hábitos de vida • Reduce la reserva fisiológica para responder al estrés Médula ósea (MO): • Aumento de la salida de neutrófilos y monocitos inflamatorios • Tráfico y proliferación de leucocitos • Aumento de la respuesta inmune mediada por células Aumento de la producción de citoquinas MCP-1,TNF α, Il-1β, IL-6 Eje Hipotálamo-Hipófisis-Adrenal (HPA) sobre regulado: CHR,Vasopresina Neuronas del núcleo paraventricular de hipotálamo Metabolismo y regulación Redox Microbioma intestinal Estado catabólico aberrante del Condrocito • Disminución de la producción ATP por mitocondrias • Aumento de producción de productos de glicación avanzados (AGE) Aumento del estrés oxidativo Disfunción endotelial • Aumento de citoquinas inflamatorias inducidas por Condrocitos • Catabolismo de la matriz extracelular (EC), Calcificación de la matriz • Aumento de la apoptosis de condrocitos Componentes bacterianos atraviesan las barreras intestinales Transfieren información entre: Intestina-SNC-células inmunesarticulación Interacción mediada por receptores: • Directa de la carga celular al huésped • Alteración de programa de expresión genética Morris Jl et al. The CNS theory of osteoarthritis: Opportunities beyond the joint. Semin Arthritis Rheum. <strong>20</strong>19 Mar 16.