DISPATCHESTable. Characteristics of family members in Ebola cluster, Bong and Montserrado Counties, Liberia, November–December 2014Date ofCity where EbolaPatient Relationship tosymptom Date admittedexposure likelyno.patient 0 Age, y/Sex Occupation onset to ETU* Outcome, date occurred†0 – 32/M Nurse’s aide Nov 14 – Died, Nov 24 Monrovia1 Father 78/M Farmer Dec 1 Dec 8 Recovered, Dec Monrovia242 Brother 39/M Auto Mechanic Dec 9 Dec 10 Recovered, Dec Monrovia233 Niece 15/F Student Dec 10 Dec 16 Recovered, Dec Monrovia304 Mother 55/F Vendor in the Dec 15 Dec 17 Died, Dec 22 Monroviamarket5 Son 3/M – Dec 16 Dec 17 Died, Dec 21 MonroviaGbarnga6 Cousin 29/F RubberplantationworkerDec 16‡ Dec 18 Recovered, Dec307 Sister§ 32/F Vendor in the Dec 18 Dec 19 Died, Dec 21 Monroviamarket8 Brother-in-law# 41/M Construction Dec 18 Dec 19 Died, Dec 27 Monroviaworker9 Niece 10/F Student Dec 20‡ Dec 20 Recovered, Jan 9 Gbarnga(2015)*ETU, Ebola treatment unit.†Gbarnga is located in Bong County; Monrovia is located in Montserrado County.‡Became symptomatic while under observation at the Bong County Holding Center.§Twin sibling of patient 0.#Husband of patient 7.The Monrovia investigation revealed that patients 1–3had contact with patient 1’s ill son, who was designated theputative source-patient (patient 0). Patient 0 was a nurse’saide at a community clinic. Fever, headache, joint pain, andabdominal pain developed in patient 0 on November 14,2014, and he was cared for at home by his family for 7 dayswhile his symptoms worsened. Although the patient andfamily members were aware of the EVD epidemic, theydid not think patient 0 had EVD because he had no vomiting,diarrhea, and hemorrhagic symptoms; they believedhe had a spiritual illness. On November 21, he was takento a church with the hope that he would be healed throughprayer. He died there on November 24, and his body wascarried to his residence for mourning and burial preparation.Because all unexplained deaths were presumed tobe Ebola related, an EVD burial crew retrieved his bodyfor cremation the following day, despite resistance fromthe family and only after persuasion by local communityleaders. No postmortem specimen was collected forEVD testing. After the body was removed, the home wassprayed with disinfectant, and the mattress, clothes, andother personal items used by patient 0 were burned. An attemptwas made to identify additional contacts; however,the family was reluctant to cooperate with health officialsand reported being angry about the cremation of patient 0and destruction of property, although these practices wereroutine at that time for controlling EVD in Monrovia. Thefamily in Monrovia began cooperating with MontserradoCounty health officials 3 weeks later, on December 18, afterlearning that 5 family members (patients 1–5) had EVDand after being provided with new mattresses and a smallration of food. At this time, they revealed 2 previously unreportedsymptomatic family members (patients 7 and 8).As of January 11, 2015, a total of 10 cases were includedin this cluster. Eight (80%) patients in this cluster were notidentified as contacts before their EVD diagnosis, and 4(40%) sought care outside the county where they resided(Table; Figure).ConclusionsIdentifying sources of infection for index patients and tracingcontacts are major components of EVD prevention andcontrol efforts (3), yet carrying out these policies is challengingwhen those ill with EVD do not reveal the names ofpossible sources or contacts who could have been exposedto disease. Detection delays and ineffective contact tracingoccurred in this cluster in part because the family believedthat the mandatory cremation and property destruction takenas public health actions in Monrovia harmed more thanhelped. Consequently, some family members sought carein Bong County, riding 4 hours in a taxi from their homein Monrovia, a distance of ≈197 kilometers. Furthermore,family members were reluctant to reveal contact names inMonrovia and initially concealed knowledge of symptomaticpersons.This cluster may have been prevented if patient 0, presumablyinfected at the clinic where he worked, had beentrained in infection control procedures and had accessto personal protective equipment. Additional exposuresand subsequent infections could have been prevented1254 Emerging Infectious Diseases • www.cdc.gov/eid • Vol. 21, No. 7, July 2015
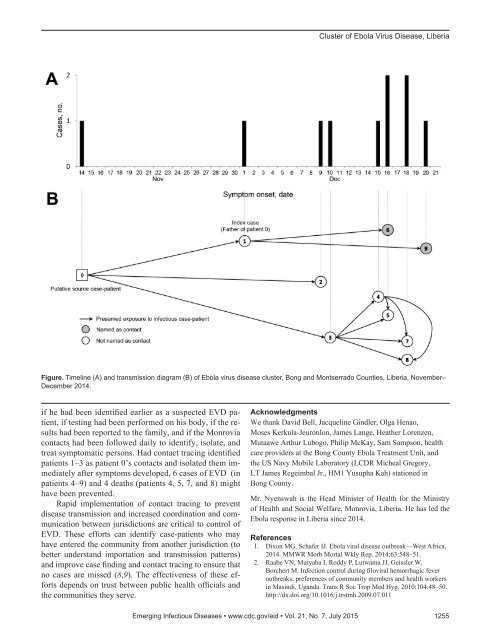
Cluster of Ebola Virus Disease, LiberiaFigure. Timeline (A) and transmission diagram (B) of Ebola virus disease cluster, Bong and Montserrado Counties, Liberia, November–December 2014.if he had been identified earlier as a suspected EVD patient,if testing had been performed on his body, if the resultshad been reported to the family, and if the Monroviacontacts had been followed daily to identify, isolate, andtreat symptomatic persons. Had contact tracing identifiedpatients 1–3 as patient 0’s contacts and isolated them immediatelyafter symptoms developed, 6 cases of EVD (inpatients 4–9) and 4 deaths (patients 4, 5, 7, and 8) mighthave been prevented.Rapid implementation of contact tracing to preventdisease transmission and increased coordination and communicationbetween jurisdictions are critical to control ofEVD. These efforts can identify case-patients who mayhave entered the community from another jurisdiction (tobetter understand importation and transmission patterns)and improve case finding and contact tracing to ensure thatno cases are missed (8,9). The effectiveness of these effortsdepends on trust between public health officials andthe communities they serve.AcknowledgmentsWe thank David Bell, Jacqueline Gindler, Olga Henao,Moses Kerkula-Jeuronlon, James Lange, Heather Lorenzen,Mutaawe Arthur Lubogo, Philip McKay, Sam Sampson, healthcare providers at the Bong County Ebola Treatment Unit, andthe US Navy Mobile Laboratory (LCDR Micheal Gregory,LT James Regeimbal Jr., HM1 Yusupha Kah) stationed inBong County.Mr. Nyenswah is the Head Minister of Health for the Ministryof Health and Social Welfare, Monrovia, Liberia. He has led theEbola response in Liberia since 2014.References1. Dixon MG, Schafer IJ. Ebola viral disease outbreak—West Africa,2014. MMWR Morb Mortal Wkly Rep. 2014;63:548–51.2. Raabe VN, Mutyaba I, Roddy P, Lutwama JJ, Geissler W,Borchert M. Infection control during filoviral hemorrhagic feveroutbreaks: preferences of community members and health workersin Masindi, Uganda. Trans R Soc Trop Med Hyg. 2010;104:48–50.http://dx.doi.org/10.1016/j.trstmh.2009.07.011Emerging Infectious Diseases • www.cdc.gov/eid • Vol. 21, No. 7, July 2015 1255
- Page 3 and 4:
July 2015SynopsisOn the CoverMarian
- Page 5 and 6:
1240 Gastroenteritis OutbreaksCause
- Page 7 and 8:
SYNOPSISDisseminated Infections wit
- Page 9 and 10:
Disseminated Infections with Talaro
- Page 11 and 12:
Disseminated Infections with Talaro
- Page 13 and 14:
Macacine Herpesvirus 1 inLong-Taile
- Page 15 and 16:
Macacine Herpesvirus 1 in Macaques,
- Page 17 and 18:
Macacine Herpesvirus 1 in Macaques,
- Page 19:
Macacine Herpesvirus 1 in Macaques,
- Page 23:
Malaria among Young Infants, Africa
- Page 26 and 27:
RESEARCHFigure 3. Dynamics of 19-kD
- Page 28 and 29:
Transdermal Diagnosis of MalariaUsi
- Page 30 and 31:
RESEARCHFigure 2. A) Acoustic trace
- Page 32 and 33:
RESEARCHof malaria-infected mosquit
- Page 34 and 35:
Lack of Transmission amongClose Con
- Page 36 and 37:
RESEARCH(IFA) and microneutralizati
- Page 38 and 39:
RESEARCHoropharyngeal, and serum sa
- Page 40 and 41:
RESEARCH6. Assiri A, McGeer A, Perl
- Page 42 and 43:
RESEARCHadvanced genomic sequencing
- Page 44 and 45:
RESEARCHTable 2. Next-generation se
- Page 46 and 47:
RESEARCHTable 3. Mutation analysis
- Page 48 and 49:
RESEARCHReferences1. Baize S, Panne
- Page 50 and 51:
Parechovirus Genotype 3 Outbreakamo
- Page 52 and 53:
RESEARCHFigure 1. Venn diagramshowi
- Page 54 and 55:
RESEARCHTable 2. HPeV testing of sp
- Page 56 and 57:
RESEARCHFigure 5. Distribution of h
- Page 58 and 59:
RESEARCHReferences1. Selvarangan R,
- Page 60 and 61:
RESEARCHthe left lobe was sampled b
- Page 62 and 63:
RESEARCHTable 2. Middle East respir
- Page 64 and 65:
RESEARCHseroprevalence in domestic
- Page 66 and 67:
RESEARCHmeasure their current surve
- Page 68 and 69:
RESEARCHTable 2. States with labora
- Page 70 and 71:
RESEARCHFigure 2. Comparison of sur
- Page 72 and 73:
RESEARCH9. Centers for Disease Cont
- Page 74 and 75:
RESEARCHthe analyses. Cases in pers
- Page 76 and 77:
RESEARCHTable 3. Sampling results (
- Page 78 and 79:
RESEARCHpresence of Legionella spp.
- Page 80 and 81:
Seroprevalence for Hepatitis Eand O
- Page 82 and 83:
RESEARCHTable 1. Description of stu
- Page 84 and 85:
RESEARCHTable 3. Crude and adjusted
- Page 86 and 87:
RESEARCHrates by gender or HIV stat
- Page 88 and 89:
RESEARCH25. Taha TE, Kumwenda N, Ka
- Page 90 and 91:
POLICY REVIEWDutch Consensus Guidel
- Page 92 and 93:
POLICY REVIEWTable 3. Comparison of
- Page 94 and 95:
POLICY REVIEW6. Botelho-Nevers E, F
- Page 96 and 97:
DISPATCHESFigure 1. Phylogenetic tr
- Page 98 and 99:
DISPATCHESSevere Pediatric Adenovir
- Page 100 and 101:
DISPATCHESTable 1. Demographics and
- Page 102 and 103:
DISPATCHES13. Kim YJ, Hong JY, Lee
- Page 104 and 105:
DISPATCHESTable. Alignment of resid
- Page 106 and 107:
DISPATCHESFigure 2. Interaction of
- Page 108 and 109:
DISPATCHESSchmallenberg Virus Recur
- Page 110 and 111: DISPATCHESFigure 2. Detection of Sc
- Page 112 and 113: DISPATCHESFigure 1. Histopathologic
- Page 114: DISPATCHESFigure 2. Detection of fo
- Page 117 and 118: Influenza Virus Strains in the Amer
- Page 119 and 120: Novel Arenavirus Isolates from Nama
- Page 121 and 122: Novel Arenaviruses, Southern Africa
- Page 123 and 124: Readability of Ebola Informationon
- Page 125 and 126: Readability of Ebola Information on
- Page 127 and 128: Patients under investigation for ME
- Page 129 and 130: Patients under investigation for ME
- Page 131 and 132: Wildlife Reservoir for Hepatitis E
- Page 133 and 134: Asymptomatic Malaria and Other Infe
- Page 135 and 136: Asymptomatic Malaria in Children fr
- Page 137 and 138: Bufavirus in Wild Shrews and Nonhum
- Page 139 and 140: Bufavirus in Wild Shrews and Nonhum
- Page 141 and 142: Range Expansion for Rat Lungworm in
- Page 143 and 144: Slow Clearance of Plasmodium falcip
- Page 145 and 146: Slow Clearance of Plasmodium falcip
- Page 147 and 148: Gastroenteritis Caused by Norovirus
- Page 149 and 150: Ebola Virus Stability on Surfaces a
- Page 151 and 152: Ebola Virus Stability on Surfaces a
- Page 153 and 154: Outbreak of Ciprofloxacin-Resistant
- Page 155 and 156: Outbreak of S. sonnei, South KoreaT
- Page 157 and 158: Rapidly Expanding Range of Highly P
- Page 159: Cluster of Ebola Virus Disease, Bon
- Page 163 and 164: ANOTHER DIMENSIONThe Past Is Never
- Page 165 and 166: Measles Epidemic, Boston, Massachus
- Page 167 and 168: LETTERSInfluenza A(H5N6)Virus Reass
- Page 169 and 170: LETTERSsystem (8 kb-span paired-end
- Page 171 and 172: LETTERS3. Van Hong N, Amambua-Ngwa
- Page 173 and 174: LETTERSTable. Prevalence of Bartone
- Page 175 and 176: LETTERSavian influenza A(H5N1) viru
- Page 177 and 178: LETTERSprovinces and a total of 200
- Page 179 and 180: LETTERS7. Manian FA. Bloodstream in
- Page 181 and 182: LETTERSforward projections. N Engl
- Page 183 and 184: LETTERS3. Guindon S, Gascuel OA. Si
- Page 185 and 186: BOOKS AND MEDIAin the port cities o
- Page 187 and 188: ABOUT THE COVERNorth was not intere
- Page 189 and 190: Earning CME CreditTo obtain credit,
- Page 191: Emerging Infectious Diseases is a p