ABSTRACTS from 16th International COnference on ... - CRRT Online
ABSTRACTS from 16th International COnference on ... - CRRT Online
ABSTRACTS from 16th International COnference on ... - CRRT Online
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<str<strong>on</strong>g>ABSTRACTS</str<strong>on</strong>g> FROM 17 TH INTERNATIONAL CONFERENCE ON <strong>CRRT</strong>,<br />
SAN DIEGO, FEB 14-17, 2012<br />
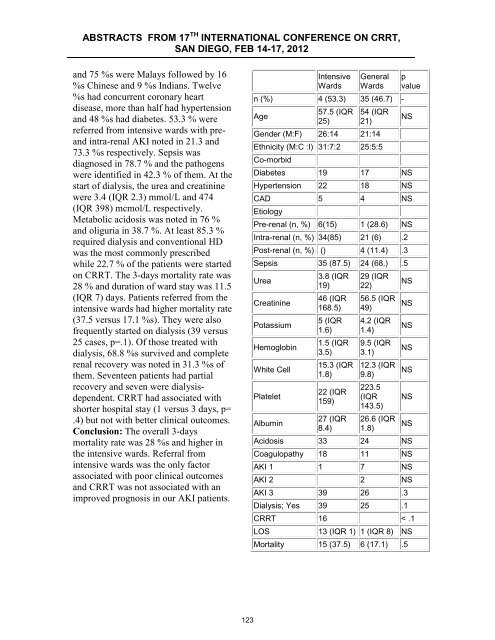
and 75 %s were Malays followed by 16<br />
%s Chinese and 9 %s Indians. Twelve<br />
%s had c<strong>on</strong>current cor<strong>on</strong>ary heart<br />
disease, more than half had hypertensi<strong>on</strong><br />
and 48 %s had diabetes. 53.3 % were<br />
referred <str<strong>on</strong>g>from</str<strong>on</strong>g> intensive wards with preand<br />
intra-renal AKI noted in 21.3 and<br />
73.3 %s respectively. Sepsis was<br />
diagnosed in 78.7 % and the pathogens<br />
were identified in 42.3 % of them. At the<br />
start of dialysis, the urea and creatinine<br />
were 3.4 (IQR 2.3) mmol/L and 474<br />
(IQR 398) mcmol/L respectively.<br />
Metabolic acidosis was noted in 76 %<br />
and oliguria in 38.7 %. At least 85.3 %<br />
required dialysis and c<strong>on</strong>venti<strong>on</strong>al HD<br />
was the most comm<strong>on</strong>ly prescribed<br />
while 22.7 % of the patients were started<br />
<strong>on</strong> <strong>CRRT</strong>. The 3-days mortality rate was<br />
28 % and durati<strong>on</strong> of ward stay was 11.5<br />
(IQR 7) days. Patients referred <str<strong>on</strong>g>from</str<strong>on</strong>g> the<br />
intensive wards had higher mortality rate<br />
(37.5 versus 17.1 %s). They were also<br />
frequently started <strong>on</strong> dialysis (39 versus<br />
25 cases, p=.1). Of those treated with<br />
dialysis, 68.8 %s survived and complete<br />
renal recovery was noted in 31.3 %s of<br />
them. Seventeen patients had partial<br />
recovery and seven were dialysisdependent.<br />
<strong>CRRT</strong> had associated with<br />
shorter hospital stay (1 versus 3 days, p=<br />
.4) but not with better clinical outcomes.<br />
C<strong>on</strong>clusi<strong>on</strong>: The overall 3-days<br />
mortality rate was 28 %s and higher in<br />
the intensive wards. Referral <str<strong>on</strong>g>from</str<strong>on</strong>g><br />
intensive wards was the <strong>on</strong>ly factor<br />
associated with poor clinical outcomes<br />
and <strong>CRRT</strong> was not associated with an<br />
improved prognosis in our AKI patients.<br />
Intensive<br />
Wards<br />
General<br />
Wards<br />
n (%) 4 (53.3) 35 (46.7) -<br />
Age<br />
57.5 (IQR<br />
25)<br />
54 (IQR<br />
21)<br />
Gender (M:F) 26:14 21:14<br />
Ethnicity (M:C :I) 31:7:2 25:5:5<br />
Co-morbid<br />
p<br />
value<br />
NS<br />
Diabetes 19 17 NS<br />
Hypertensi<strong>on</strong> 22 18 NS<br />
CAD 5 4 NS<br />
Etiology<br />
Pre-renal (n, %) 6(15) 1 (28.6) NS<br />
Intra-renal (n, %) 34(85) 21 (6) .2<br />
Post-renal (n, %) () 4 (11.4) .3<br />
Sepsis 35 (87.5) 24 (68.) .5<br />
Urea<br />
Creatinine<br />
Potassium<br />
Hemoglobin<br />
White Cell<br />
Platelet<br />
Albumin<br />
3.8 (IQR<br />
19)<br />
46 (IQR<br />
168.5)<br />
5 (IQR<br />
1.6)<br />
1.5 (IQR<br />
3.5)<br />
15.3 (IQR<br />
1.8)<br />
22 (IQR<br />
159)<br />
27 (IQR<br />
8.4)<br />
29 (IQR<br />
22)<br />
56.5 (IQR<br />
49)<br />
4.2 (IQR<br />
1.4)<br />
9.5 (IQR<br />
3.1)<br />
12.3 (IQR<br />
9.8)<br />
223.5<br />
(IQR<br />
143.5)<br />
26.6 (IQR<br />
1.8)<br />
NS<br />
NS<br />
NS<br />
NS<br />
NS<br />
NS<br />
NS<br />
Acidosis 33 24 NS<br />
Coagulopathy 18 11 NS<br />
AKI 1 1 7 NS<br />
AKI 2 2 NS<br />
AKI 3 39 26 .3<br />
Dialysis; Yes 39 25 .1<br />
<strong>CRRT</strong> 16 < .1<br />
LOS<br />
13 (IQR 1) 1 (IQR 8) NS<br />
Mortality 15 (37.5) 6 (17.1) .5<br />
123