Invasive breast carcinoma - IARC
Invasive breast carcinoma - IARC
Invasive breast carcinoma - IARC
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
schema {1535,2602}. Although this classification<br />
has been widely applied, its<br />
reproducibility is somewhat disappointing<br />
{240,1433}, and molecular data with<br />
direct implications for histological diagnosis<br />
were unavailable at the time of the<br />
1994 classification {1956}. Nevertheless,<br />
it remains the best available classification<br />
and has been adopted in this new<br />
edition.<br />
Endometrial hyperplasias are assumed<br />
to evolve as a progressive spectrum of<br />
endometrial glandular alterations divided<br />
into four separate categories by architecture<br />
and cytology. The vast majority of<br />
endometrial hyperplasias mimic proliferative<br />
endometria, but rare examples<br />
demonstrate secre t o ry features. The<br />
entire spectrum of metaplastic changes<br />
may be observed in hyperplastic<br />
endometria.<br />
Hyperplasias without atypia<br />
Hyperplasias without atypia re p re s e n t<br />
the exaggerated proliferative response<br />
to an unopposed estrogenic stimulus;<br />
the endometrium responds in a diffuse<br />
manner with a balanced increase of both<br />
glands and stroma. In simple hyperplasia<br />
the glands are tubular although frequently<br />
cystic or angular, and some even<br />
show minor epithelial budding. The lining<br />
is pseudostratified with cells displaying<br />
regular, elongated nuclei lacking atypia.<br />
In complex (adenomatous) hyperplasia<br />
the glands display extensive complicated<br />
architectural changes represented by<br />
i r regular epithelial budding into both<br />
lumina and stroma and a typical cytology<br />
with pseudostratified but uniform, elongated<br />
and polarized glandular nuclei;<br />
squamous epithelial morules can be<br />
present. There is most often a shift in the<br />
gland to stroma ratio in favour of the<br />
glands.<br />
Atypical hyperplasias<br />
The main feature which differentiates this<br />
category from the previous one is the<br />
atypical cytology of the glandular lining<br />
as represented by loss of axial polarity,<br />
unusual nuclear shapes that are often<br />
rounded, irregularity in the nuclear membranes,<br />
prominent nucleoli and cleared<br />
or dense chromatin. Atypia occurs nearly<br />
always focally.<br />
Simple atypical hyperplasia feature s<br />
atypical glandular cytology superimposed<br />
on the arc h i t e c t u re of simple<br />
hyperplasia. This pattern is extremely<br />
unusual. The frequently found complex<br />
atypical (adenomatous with atypia)<br />
hyperplasia is a lesion characterized by<br />
an increased glandular complexity with<br />
i r regular outgrowths and cytological<br />
atypia. There may be associated foci of<br />
non-endometrioid differentiation such as<br />
squamous morules. Due to the expansion<br />
and crowding of glands, the interglandular<br />
stroma is diminished but<br />
remains present. Characteristic features<br />
of adeno<strong>carcinoma</strong> are absent.<br />
The assessment of cytological atypia is<br />
the key problem in assigning individual<br />
cases to one of the four different WHO<br />
categories. Definitions of cytological<br />
atypia are difficult to apply in the<br />
endometrium because nuclear cytological<br />
changes occur frequently in hormonal<br />
imbalance, benign regeneration and<br />
metaplasia {1619,2033}. Paradoxically,<br />
atypical hyperplasia may exhibit more<br />
atypical features than adeno<strong>carcinoma</strong><br />
{2688}, and some grade 1 invasive<br />
endometrioid <strong>carcinoma</strong>s have an<br />
e x t remely bland cytology. Perhaps, it<br />
would be more appropriate to consider<br />
cytological changes in the context of<br />
overall glandular architecture. Indeed,<br />
architectural focality of the lesion is so<br />
closely linked with atypia that possibly<br />
they are inseparable. In this way, atypia<br />
is best observed by comparison with<br />
adjoining normal glands.<br />
Caveat: sampling problems<br />
The focal nature of atypical endometrial<br />
hyperplasias may allow young women to<br />
maintain fertility, but has the disadvantage<br />
of possible underdiagnosis due to<br />
incomplete sampling. The problem is<br />
g reatest in scanty fragmented specimens,<br />
something commonly encountered<br />
in routine office biopsies. Clearly,<br />
this situation is responsible for the false<br />
negative biopsies during follow up.<br />
Hysteroscopic direction may assist in targeting<br />
a macroscopically apparent localized<br />
lesion but is not a common practice<br />
in most settings.<br />
Contemporary approach to<br />
endometrial hyperplasia<br />
Poor reproducibility of the 1994 WHO<br />
hyperplasia schema {240,1433} has led<br />
to a proposal to reduce the number of<br />
diagnostic classes {240}. New concepts<br />
of pathogenesis have been incorporated<br />
into an integrated genetic, histomorphometric<br />
and clinical outcome model of<br />
A<br />
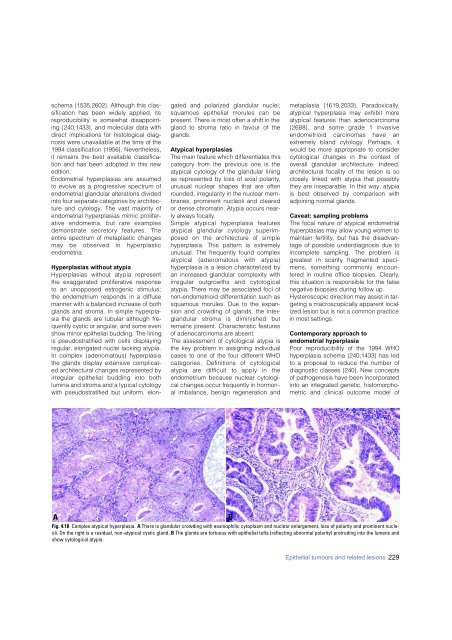
Fig. 4.18 Complex atypical hyperplasia. A There is glandular crowding with eosinophilic cytoplasm and nuclear enlargement, loss of polarity and prominent nucleoli.<br />
On the right is a residual, non-atypical cystic gland. B The glands are tortuous with epithelial tufts (reflecting abnormal polarity) protruding into the lumens and<br />
show cytological atypia.<br />
B<br />
Epithelial tumours and related lesions 229