LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Clinical symptom index More symptoms<br />
1.0<br />
0.9<br />
0.8<br />
0.7<br />
0.6<br />
0.5<br />
0.4<br />
+<br />
-<br />
Neuropsychological vulnerability index<br />
+ +<br />
+<br />
Biological principles <strong>of</strong> <strong>the</strong> risk <strong>of</strong> illness<br />
for psychotic disorders<br />
Participation in <strong>the</strong> homonymous, multi-centre project<br />
<strong>of</strong> <strong>the</strong> Competence Network on Schizophrenia (Principal<br />
investigator: M. Wagner, <strong>University</strong> <strong>of</strong> Bonn)<br />
W. Wölwer, M. Streit, J. Brinkmeyer, S. Stroth<br />
Project period: 2000–2006<br />
Financing: FMER funding 01 GI 9934, 01 GI 0234 to<br />
Wagner, Bonn<br />
This sub-project aims, amongst o<strong>the</strong>r things, to test<br />
whe<strong>the</strong>r neuropsychological indicators <strong>of</strong> increased<br />
vulnerability to psychosis can contribute to predicting <strong>the</strong><br />
actual development <strong>of</strong> a psychotic disorder in persons<br />
who have been identified using clinical criteria as at-risk<br />
groups (Figure 9). Known neuropsychological vulnerability<br />
indicators were assessed in at-risk persons in <strong>the</strong> assumed<br />
early and late prodromal stages <strong>of</strong> a psychotic development<br />
both at inclusion into one <strong>of</strong> <strong>the</strong> early diagnosis and early<br />
intervention projects <strong>of</strong> <strong>the</strong> Competence Network and after<br />
twelve months. Compared with healthy controls <strong>the</strong> risk<br />
group in <strong>the</strong> late prodromal stage demonstrated statistically<br />
-<br />
+ + + +<br />
+<br />
+<br />
++<br />
+<br />
-<br />
-<br />
- -<br />
-<br />
-<br />
- - --<br />
--<br />
-<br />
-<br />
-<br />
-<br />
-<br />
- --<br />
-<br />
++ +<br />
+ +<br />
++<br />
+<br />
+<br />
+ ++ + +<br />
+<br />
++ +<br />
++ ++ +++ +++<br />
+<br />
+<br />
+++++<br />
+<br />
+<br />
+<br />
+<br />
0.4 0.5 0.6 0.7 0.8 0.9 1.0<br />
+<br />
+<br />
Increased vulnerability<br />
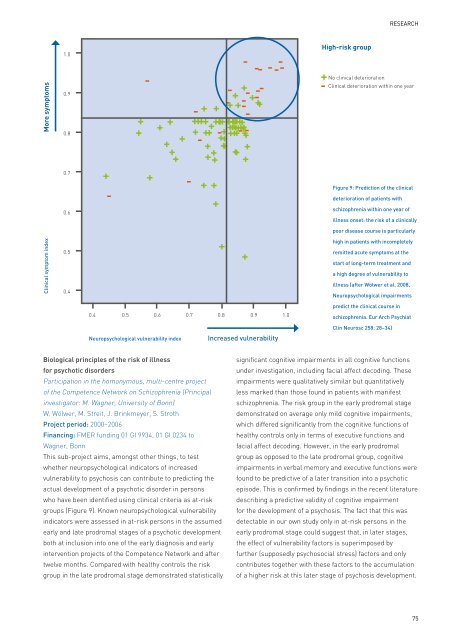
High-risk group<br />
- +<br />
ReseaRch<br />
No clinical deterioration<br />
Clinical deterioration within one year<br />
Figure 9: Prediction <strong>of</strong> <strong>the</strong> clinical<br />
deterioration <strong>of</strong> patients with<br />
schizophrenia within one year <strong>of</strong><br />
illness onset: <strong>the</strong> risk <strong>of</strong> a clinically<br />
poor disease course is particularly<br />
high in patients with incompletely<br />
remitted acute symptoms at <strong>the</strong><br />
start <strong>of</strong> long-term treatment and<br />
a high degree <strong>of</strong> vulnerability to<br />
illness (after Wölwer et al. 2008,<br />
Neuropsychological impairments<br />
predict <strong>the</strong> clinical course in<br />
schizophrenia. Eur Arch Psychiat<br />
Clin Neurosc 258: 28–34)<br />
significant cognitive impairments in all cognitive functions<br />
under investigation, including facial affect decoding. These<br />
impairments were qualitatively similar but quantitatively<br />
less marked than those found in patients with manifest<br />
schizophrenia. The risk group in <strong>the</strong> early prodromal stage<br />
demonstrated on average only mild cognitive impairments,<br />
which differed significantly from <strong>the</strong> cognitive functions <strong>of</strong><br />
healthy controls only in terms <strong>of</strong> executive functions and<br />
facial affect decoding. However, in <strong>the</strong> early prodromal<br />
group as opposed to <strong>the</strong> late prodromal group, cognitive<br />
impairments in verbal memory and executive functions were<br />
found to be predictive <strong>of</strong> a later transition into a psychotic<br />
episode. This is confirmed by findings in <strong>the</strong> recent literature<br />
describing a predictive validity <strong>of</strong> cognitive impairment<br />
for <strong>the</strong> development <strong>of</strong> a psychosis. The fact that this was<br />
detectable in our own study only in at-risk persons in <strong>the</strong><br />
early prodromal stage could suggest that, in later stages,<br />
<strong>the</strong> effect <strong>of</strong> vulnerability factors is superimposed by<br />
fur<strong>the</strong>r (supposedly psychosocial stress) factors and only<br />
contributes toge<strong>the</strong>r with <strong>the</strong>se factors to <strong>the</strong> accumulation<br />
<strong>of</strong> a higher risk at this later stage <strong>of</strong> psychosis development.<br />
75