LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
LVR-Klinikum Düsseldorf Hospital of the Heinrich-Heine University ...
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>LVR</strong>-KLINIKUM DÜsseLDORF – hOsPITaL OF The heINRIch-heINe UNIVeRsITY DÜsseLDORF<br />
Biological principles <strong>of</strong> relapse in schizophrenia<br />
Participation in <strong>the</strong> homonymous multi-centre project<br />
within <strong>the</strong> Competence Network on Schizophrenia (Principal<br />
investigators: W. Gaebel and W. Wölwer)<br />
W. Wölwer, M. Streit, J. Brinkmeyer, W. Gaebel<br />
Project period: 2000–2006<br />
Financing: FMER funding 01 GI 9932, 01 GI 0232<br />
Using <strong>the</strong> vulnerability-stress-coping model <strong>of</strong> schizophrenia<br />
as a starting point, <strong>the</strong> three components <strong>of</strong> this model were<br />
assessed in 125 first-episode patients with schizophrenia<br />
at <strong>the</strong> start and after <strong>the</strong> first and second year <strong>of</strong> longterm<br />
treatment in order to investigate <strong>the</strong>ir contribution<br />
to <strong>the</strong> risk <strong>of</strong> relapse as well as <strong>the</strong>ir relationship with <strong>the</strong><br />
occurrence <strong>of</strong> prodromal symptoms and severe clinical<br />
deterioration.<br />
The study showed that patients with later clinical<br />
deterioration demonstrate stronger cognitive impairments in<br />
executive functions before <strong>the</strong> start <strong>of</strong> long-term treatment<br />
than patients with relatively stable clinical remission. Such<br />
cognitive impairments prove to be significant predictors<br />
<strong>of</strong> clinical development in regression analyses, even<br />
exceeding in predictive validity clinical variables such as<br />
<strong>the</strong> remaining positive symptoms at <strong>the</strong> start <strong>of</strong> long-term<br />
treatment. However, <strong>the</strong>y demonstrate only low sensitivity<br />
(72%) and specificity (51%), which clearly restricts <strong>the</strong>ir use<br />
for individual risk predictions. In this regard, combinations<br />
<strong>of</strong> <strong>the</strong> neuropsychological (executive functions) and clinical<br />
parameters (residual symptoms) taken from <strong>the</strong> start <strong>of</strong><br />
long-term treatment were superior, ins<strong>of</strong>ar as only <strong>the</strong> risk,<br />
not <strong>the</strong> time <strong>of</strong> clinical deterioration was to be predicted.<br />
To predict <strong>the</strong> time when such a deterioration could occur,<br />
unspecific prodromal symptoms – assessed fortnightly<br />
during <strong>the</strong> course <strong>of</strong> <strong>the</strong> long-term treatment – proved to be<br />
<strong>the</strong> superior predictors.<br />
24<br />
22<br />
20<br />
18<br />
16<br />
14<br />
76<br />
Number <strong>of</strong> correct responses in a<br />
standardised test <strong>of</strong> facial affect recognition<br />
Training <strong>of</strong> affect decoding<br />
Cognitive remediation training<br />
No training<br />
T 0 T1<br />
Before training After training<br />
Psychological intervention strategies in<br />
cognitive and emotional disorders<br />
W. Wölwer, N. Frommann, S. Halfmann, M. Streit in<br />
cooperation with R. Vauth (<strong>University</strong> <strong>of</strong> Freiburg/Basel)<br />
Project period: 2000–2003<br />
Financing: FMER funding 01 GI 9932<br />
Impairments in social-cognitive processes, such as facial<br />
affect decoding, are well documented in people with<br />
schizophrenia, are stable across <strong>the</strong> course <strong>of</strong> <strong>the</strong> disorder<br />
and make a significant contribution to <strong>the</strong> <strong>of</strong>ten poor<br />
social functioning <strong>of</strong> people with schizophrenia. Since <strong>the</strong><br />
impairments remain largely uninfluenced by <strong>the</strong> usual<br />
treatment strategies, <strong>the</strong> search remains for alternative<br />
treatment approaches. For this reason, <strong>the</strong> Training <strong>of</strong><br />
Affect Recognition (TAR) was newly developed in <strong>the</strong><br />
Experimental Psychopathology Research Laboratory. The<br />
TAR was first evaluated with regard to potential increases<br />
in performance in facial affect recognition in a randomised<br />
pre-post control group design in comparison with an active<br />
control condition (basic-cognitive remediation training [CRT]<br />
for <strong>the</strong> improvement <strong>of</strong> neurocognitive basic functions) and<br />
compared with usual treatment (Treatment as Usual [TAU])<br />
without any additional cognitive training (Figure 10). At <strong>the</strong><br />
same time, such “molecular” training approaches focusing<br />
on circumscribed cognitive functions were compared with<br />
broader “molar” training strategies addressing a number <strong>of</strong><br />
cognitive and behaviour-related functions. Altoge<strong>the</strong>r, <strong>the</strong><br />
results produced a picture <strong>of</strong> a double dissociation, in which<br />
social-cognitive training strategies improve facial affect<br />
decoding, but do not improve memory performance, whereas<br />
basic-cognitive training improves memory, but not affect<br />
decoding. Both effects were achieved almost independently<br />
<strong>of</strong> <strong>the</strong> type <strong>of</strong> training strategy (molar vs. molecular) that was<br />
used for <strong>the</strong> respective area. Correspondingly, impairments<br />
<strong>of</strong> facial affect decoding in people with schizophrenia can<br />
in general be treated if training strategies that specifically<br />
address social-cognitive functions are used.<br />
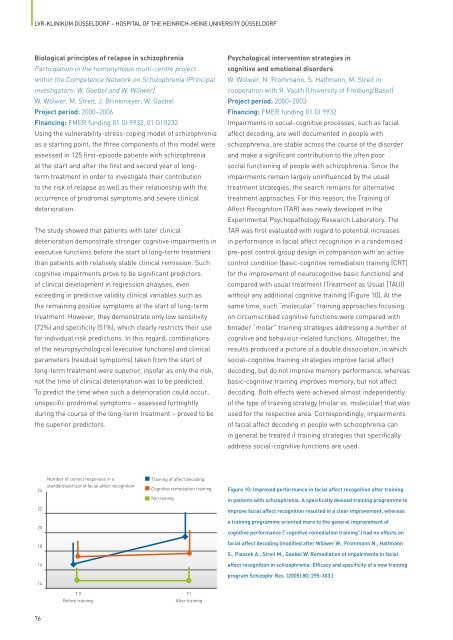
Figure 10: Improved performance in facial affect recognition after training<br />
in patients with schizophrenia. A specifically devised training programme to<br />
improve facial affect recognition resulted in a clear improvement, whereas<br />
a training programme oriented more to <strong>the</strong> general improvement <strong>of</strong><br />
cognitive performance (“cognitive remediation training”) had no effects on<br />
facial affect decoding (modified after Wölwer W., Frommann N., Halfmann<br />
S., Piaszek A., Streit M., Gaebel W. Remediation <strong>of</strong> impairments in facial<br />
affect recognition in schizophrenia: Efficacy and specificity <strong>of</strong> a new training<br />
program Schizophr Res. (2005) 80; 295-303.)