Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Sie wollen auch ein ePaper? Erhöhen Sie die Reichweite Ihrer Titel.
YUMPU macht aus Druck-PDFs automatisch weboptimierte ePaper, die Google liebt.
S78<br />
Abstracts<br />
monitored by measuring the proteoglycan release into the supernatant<br />
(DMB-assay) and by Safranin-O-staining of histological sections. Total<br />
MMP-activity in the supernatant was quantifi ed using a fl uorescence assay<br />
with a broadly MMP-specifi c peptide substrate. Classifi cation of the<br />
individual MMP‘s was achieved by gelatine zymography. Morphology<br />
of SF and cartilage surface was examined by raster electron microscopy<br />
(REM). Results:For all stimuli proteoglycan release following co-culture<br />
of BC with RA-, OA- and JT-SF was quantitatively higher than in<br />
the corresponding BC-monoculture. In BC-monoculture stimulation<br />
with IL-1β or IL-1β/TNF-α, but not TNF-α alone, signifi cantly increased<br />
proteoglycan depletion as compared to non stimulated controls.<br />
In co-culture with RA-, OA-, or JT-SF, however all stimulations led to<br />
signifi cantly higher proteoglycan release compared to non-stimulated<br />
controls. Interestingly, signifi cantly higher levels of total MMP-activity<br />
were observed for all stimuli in both BC-monoculture and co-culture<br />
with RA-, OA- and JT- SF. Quantitatively however, the total MMP-activity<br />
in stimulated co-cultures showed up to 4 fold higher levels compared<br />
with BC-monoculture. In zymography cytokine treated BC-monocultures<br />
and co-cultures with SF showed an increased MMP-2 and<br />
MMP-9 activity, though co-cultures led to distinct higher values than<br />
BC-monoculture. REM revealed that cytokine treatment induced: i)<br />
degradation of the cartilage matrix already in BC-monoculture; and ii)<br />
an activated phenotype of SF in co-culture.<br />
Conclusion: Stimulation with TNF-α, IL-1β or TNF-α/IL-1β results in<br />
increased cartilage degradation and MMP-activity in both BC-monoculture<br />
and co-culture with SF. Signifi cantly or numerically increased<br />
overall MMP-, MMP-2-, and MMP-9 activity following co-culture with<br />
SF, on the other hand, underlines the central role of SF for cartilage<br />
degradation. Comparison of the 2 culture systems may allow to distinguish<br />
the relative contribution of BC and SF to cartilage degradation.<br />
POFER-12<br />
Striktly time-dependent regulation of the mRNA expression<br />
of pro-infl ammatory/pro-destructive genes in sfb by TNF-alpha<br />
Kunisch E., Gandesiri M., Lux S., Jansen A., Kinne RW.<br />
Nachwuchsgruppe Experimentelle <strong>Rheumatologie</strong>, Friedrich-Schiller-Universität<br />
Jena<br />
Purpose: TNF-alpha is a major inductor of pro-destructive/pro-infl<br />
ammatory processes in rheumatoid arthritis (RA), whose infl uence<br />
on RA synovial fi broblast (SFB) functions has been extensively studied.<br />
However, there are limited data about the time-dependent induction<br />
of these functions by TNF-alpha. Th erefore, the present study sought<br />
to characterize the time-dependent induction of mRNA expression for<br />
MMP-1, MMP-3, COX2, IL-8 and IL-6 in RA-, osteoarthritic (OA)-,<br />
and joint trauma (JT)-SFB following TNF-alpha stimulation.<br />
Methods: For analysis of time-dependent mRNA expression for MMP-<br />
1, MMP-3, COX2, IL-8, and IL-6, RA-, OA-, and JT-SFB (beginning of<br />
3rd passage) were stimulated with TNF-alpha (10 ng/ml) for 0, 1, 2, 4, 6,<br />
8, 10, and 24 h. mRNA expression was analyzed by real-time RT-PCR.<br />
Results: COX2 and IL-6 mRNA reached their maxima 1h aft er TNFalpha<br />
stimulation, with a strong decrease until about 8 h and a slight<br />
increase thereaft er. IL-8 mRNA was also induced aft er 1 h stimulation<br />
but had a maximum following 4<strong>–</strong>8 h TNF-alpha stimulation. In contrast,<br />
MMP-1 and MMP-3 mRNA expression showed a continuous increase<br />
in RA-, OA-, and JT-SFB over the 24 h period of TNF-alpha<br />
stimulation.<br />
Conclusions: Time-dependent induction of mRNA for the pro-destructive/pro-infl<br />
ammatory molecules MMP-1, MMP3, COX2, IL-8<br />
and IL-6 was observed in RA-, OA-, and JT-SFB following TNF-alpha<br />
stimulation. Whereas pro-infl ammatory molecules showed their maximal<br />
mRNA expression as early as 1h, pro-destructive molecules did<br />
not reach their maxima until 24 h aft er TNF-alpha stimulation. Th ese<br />
data show a strictly time-dependent, possibly cascade-signal regulated<br />
mRNA expression for pro-destructive/pro-infl ammatory molecules in<br />
| <strong>Zeitschrift</strong> <strong>für</strong> <strong>Rheumatologie</strong> · <strong>Supplement</strong> 1 · 2006<br />
RA, OA-, and JT-SFB following TNF-alpha stimulation with potential<br />
relevance for pathophysiological and therapeutic aspects.<br />
Th is study was supported by the German Federal Ministry of Education<br />
and Research (BMBF; grant FKZ 01ZZ0105 to R.W. Kinne, Interdisciplinary<br />
Center for Clinical Research Jena) and the German Research<br />
Foundation (DFG; grant KI 439/7-1 to R.W. Kinne), as well as a<br />
grant for the advancement of female scientists to E. Kunisch (LUBOM<br />
Th uringia 05/2005-05/2005).<br />
POFER-13<br />
Low baseline serum cortisol predicts marked clinical improvement<br />
7 days after initiation of anti-TNF antibody therapy in rheumatoid<br />
arthritis<br />
Straub RH. 1 , Härle P. 1 , Pongratz G. 1 , Fleck M. 1 , Cutolo M. 2 , Atzeni F. 3 ,<br />
Antoni C. 4 , Kalden JR. 5 , Lorenz HM. 6 , Sarzi-Puttini P. 3<br />
1 Laboratory of Exp. Rheumatology and Neuroendocrino-Immunology,<br />
Dept. of Internal Medicine I, University Hospital Regensburg, 93042<br />
Regensburg, Germany, 2 Division of Rheumatology, Department of Internal<br />
Medicine and Medical Specialties, University of Genova, Italy, 3 Rheumatology<br />
Unit, University Hospital L Sacco, Milan, Italy, 4 Schering-Plough<br />
Research Institute, Kenilworth, NJ 07033, U.S.A., 5 Dept. of Internal Medicine<br />
III, University of Erlangen<strong>–</strong>Nürnberg, 91054 Erlangen, Germany, 6 Division<br />
of Rheumatology, Dept. of Internal Medicine V, University of Heidelberg,<br />
69120 Heidelberg, Germany<br />
Objective: It is known clinical experience that some patients with rheumatoid<br />
arthritis (RA) rapidly profi t from anti-TNF antibody therapy<br />
whereas others show no immediate benefi t. Th is investigation studied<br />
the predictive role of hypothalamic <strong>–</strong> pituitary <strong>–</strong> adrenal (HPA) axis<br />
hormones for immediate clinical improve-ment during anti-TNF antibody<br />
therapy.<br />
Methods: In this study in 24 RA patients, we measured at baseline adrenocorticotropic<br />
hormone (ACTH), 17-hydroxyprogesterone (17OHP),<br />
cortisol, and interleukin (IL)-6. Immediate clinical improve-ment was<br />
judged 7 days aft er initiation of therapy by the physician global estimate<br />
of disease activity, which appraises pain, well-being, and functional<br />
ability.<br />
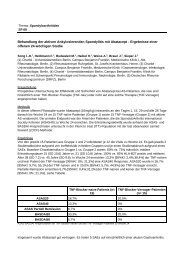
Results: Compared to patients with little improvement, patients with<br />
>50% improvement were not diff erent in age, gender, accompanying<br />
therapies, and <strong>–</strong> at baseline <strong>–</strong> physician global assessment, ESR, serum<br />
IL-6 and ACTH. However, patients with > 50% improvement had lower<br />
baseline serum levels of cortisol and a lower baseline ratio of serum<br />
cortisol divided by serum 17OHP. Th e extent of improvement negatively<br />
correlated with baseline serum cortisol (R=-0.457, p=0.025) and<br />
the cortisol/17OHP ratio (R=-0.589, p=0.003). In the longitudinal part<br />
of this study over 12 weeks, those patients with >50% improve-ment<br />
demonstrated steadily increasing serum levels of cortisol, which was<br />
not observed in patients with little improvement.<br />
Conclusions: Since TNF inhibits adrenal conversion of 17OHP into<br />
cortisol leading to low serum corti-sol, these fi ndings indicate that<br />
some patients rapidly profi t from TNF neutralization probably by restoring<br />
this important enzyme step. In responders, TNF neutralization<br />
leads to an increase in serum cortisol and rapid clinical improvement.