Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Zeitschrift für Rheumatologie – Supplement 1 - Deutsche ...
Erfolgreiche ePaper selbst erstellen
Machen Sie aus Ihren PDF Publikationen ein blätterbares Flipbook mit unserer einzigartigen Google optimierten e-Paper Software.
teins along with lineage, activation and migration markers, cytokine<br />
and complement receptors. Finally we present a prototype of a database<br />
necessary for data storage and data analysis.<br />
In summary, the approach presented provides a powerful platform for<br />
validation of candidate genes at the protein level and their monitoring<br />
for clinical applications.<br />
POFER-21<br />
Genetic Association of Progressive Systemic Sclerosis (SSc) with<br />
PTPN22 Polymorphisms<br />
Kirsten H. 1 *, Ahnert P. 1 *, Dümmler J. 2 , Hunzelmann N. 3 , Vaith P. 4 , Melchers I. 2<br />
1 2 Universität Leipzig, IKIT/BBZ, Klinische Forschergruppe <strong>für</strong> <strong>Rheumatologie</strong>,<br />
Universitätsklinikum Freiburg,<br />
3 Universitätshautklinik Köln,<br />
4 <strong>Rheumatologie</strong> und Klin. Immunologie, Universitätsklinikum Freiburg<br />
*contributed equally<br />
Recently, associations between type I diabetes, rheumatoid arthritis<br />
as well as several other autoimmune diseases (AIDs) and the PTPN22<br />
single nucleotide polymorphism (SNP) 1858C→T were discovered.<br />
PTPN22 (encoding protein tyrosine phosphatase, non-receptor type<br />
22) located on chromosome 1p13 has 21 exons spanning 58 kb. Th e<br />
variant 1858C→T in codon 620 results in the exchange of Arg to Trp<br />
(R620W). PTPN22 (also known as Lyp or Pep) is expressed primarily<br />
in lymphoid tissue, and most probably involved in the negative regulation<br />
of T cell activation via interaction with the protein tyrosine kinase<br />
Csk. It was suggested that the mutation 620W may interfere with the<br />
interaction between Lyp and Csk. However, functional data comparing<br />
homozygous and heterozygous 620W carriers are not yet available.<br />
We collected DNA from 177 patients with SSc and 184 healthy blood<br />
donors (HD). Samples were analyzed for 13 SNPs covering PTPN22,<br />
including 1858C→T (rs2476601). SNPs were selected to represent the<br />
most common haplotypes. Th e analysis was performed by PCR, single<br />
base extension and MALDI-TOF mass spectrometry.<br />
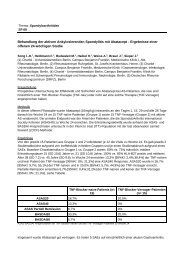
Among HD, the allele frequency of 1858T was 9.0 %, similar to published<br />
data. Genotype frequency of 1858T/T was 0.5 %. Among SSc patients,<br />
the allele frequency of 1858T was 12.4 %, genotype frequency of<br />
1858T/T was 2.8 %. Th e diff erence in allele frequencies did not reach<br />
statistical signifi cance, however, the diff erence in genotype frequencies<br />
was signifi cant (p = 0.01, genotype relative risk test, Lathrop. Tissue<br />
Antigens. 1983; 22:160<strong>–</strong>166). Data concerning subgroups of patients,<br />
additional polymorphisms and the other 4 major haplotypes of<br />
PTPN22, together accounting for about 98.5 % of detectable variants,<br />
will also be discussed.<br />
So far, associations observed in AIDs with PTPN22 always only concerned<br />
a subpopulation of patients since only a subset of the patients<br />
carried the disease associated variant. For PTPN22, maximally 20 % of<br />
AID patients were shown to carry the allele 1858T and even less carried<br />
the homozygous 1858T/T genotype. Th erefore, only a small subpopulation<br />
of patients may be infl uenced by functional eff ects due to PTPN22.<br />
In SSc patients, this subpopulation may be quite small, but it does exist.<br />
Supported by grants of the BMBF (“German Network for Systemic Scleroderma”<br />
to IM and NH, “University and Science” to PA), the Sächsische<br />
Aufb aubank (PA) and the EFRE (PA).<br />
POFER-22<br />
Cyclophosphamide reduces cellular infi ltrates in the infl amed<br />
kidneys rather than aff ecting lymphoproliferation or auto-antibody<br />
levels in a murine model of lupusnephritis<br />
Humrich JY. 1 , Schürer S. 2 , Wittenburg G. 2 , Enghard P. 1 , Undeutsch R. 1 ,<br />
Berek C. 2 , Riemekasten G. 1<br />
1 <strong>Rheumatologie</strong> und Klinische Immunologie, Charité Berlin, 2 DRFZ Berlin<br />
Cyclophosphamide is commonly used as a standard therapy for the<br />
treatment of lupusnephritis. Based on its DNA-alkylating properties it<br />
is assumed that the benefi cial eff ect of cyclophospamide is due to the<br />
inhibition of proliferation of autoreactive T and B cells in secondary<br />
lymphoid organs, which results in a decreased generation of nephritogenic<br />
auto-antibodies. We used the (NZBxNZW) F1 lupus model to<br />
evaluate the eff ects of a cyclophospamide pulse-therapy on kidney infl<br />
ammation and cellular activity in secondary lymphoid organs. Mice<br />
were treated daily with 1mg of cyclophosphamide or as control with<br />
PBS for the duration of one week. Sera were collected before and aft er<br />
treatment, and the proteinuria was simultaneously determined. Th ree<br />
weeks and fi ve weeks aft er therapy kidneys and spleens were isolated<br />
from fi ve mice in each group. Th e phenotype and activation status of<br />
splenic CD4+ T cells and B cell subpopulation were examined by fl ow<br />
cytometry. Kidneys and one part of the spleens were prepared for immunohistological<br />
analyses. Sera were screened for anti-ds-DNA antibody<br />
levels by ELISA. Treatment with cyclophosphamide signifi cantly<br />
reduced proteinuria almost to normal levels and signifi cantly prolonged<br />
the survival of the treated group. Immunohistological analysis of<br />
kidney sections showed a marked reduction of the cellular infi ltrate<br />
in parallel to the reduction of proteinuria. In contrast, we found only<br />
moderate eff ects on the phenotype of splenic CD4+ T cell with a slight<br />
decrease of CD69+ cells and an increase of CD62L+ cells, while no<br />
changes in the frequencies of splenic CD138+ plasmablasts, CD23+ follicular<br />
B cells, CD21+ marginal zone B cells or PNA++ germinal center<br />
B cells could be observed. Complementary to this histological analysis<br />
of the spleens showed only moderate eff ects on the architecture and the<br />
size of the lymphoid follicles. Most interestingly we could not detect a<br />
reduction of the serum anti-ds-DNA antibody levels aft er treatment.<br />
Th us we conclude that cyclophophamide interacts directly with kidney<br />
infi ltrating cells at the site of infl ammation rather than aff ecting proliferation<br />
of autoreactive T and B cells in secondary lymphoid organs.<br />
Furthermore we suggest that auto-antibodies and humoral immunity<br />
might not be such relevant for lupusnephritis, since improvement of<br />
nephritis was achieved despite the presence of high levels of anti-ds-<br />
DNA antibodies in the sera aft er treatment with cyclophosphamide.<br />
POFER-23<br />
Das Wegener Autoantigen Proteinase 3 (PR3) in Organo- und<br />
Pathogenese<br />
Relle M., Galle PR., Schwarting A.<br />
I. Medizinische Klinik und Poliklinik, Uniklinikum Mainz, Mainz<br />
Zielsetzung: Die Proteinase 3 (PR3) ist eine neutrale Serin-Protease<br />
Neutrophiler Granulozyten, Mastzellen und Monozyten. Sie ist auch<br />
als Myeloblastin, ein Wachstumsfaktor myeloider Zellen, bekannt.<br />
Rahmen der Wegenerschen Granulomatose ist die PR3 das Hauptzielantigen<br />
antineutrophiler cytoplasmatischer Autoantikörper (c-<br />
ANCA). Nach wie vor kontrovers diskutiert wird die Expression der<br />
PR3 in non-myeloiden Zellen, obwohl sie zweifelsfrei im Endothel, in<br />
Nierenzellen und in epithelialen Tumorzell-Linien nachgewiesen werden<br />
konnte.<br />
Methoden: Da das Expressionsprofi l der PR3 im Bezug auf die Pathophysiologie<br />
von Autoimmunerkrankungen, wie z. B. dem Morbus Wegener<br />
von essentieller Bedeutung ist, wurden Dot Blot- und Northern<br />
Blot-Analysen durchgeführt, um PR3-Transkripte in verschiedenen<br />
Organen, Tumoren und Tumorzell-Linien zu detektieren. Ferner wurden<br />
PR3-spezifi sche Primer eingesetzt, um PR3-Transkripte sowohl in<br />
<strong>Zeitschrift</strong> <strong>für</strong> <strong>Rheumatologie</strong> · <strong>Supplement</strong> 1 · 2006 | S81